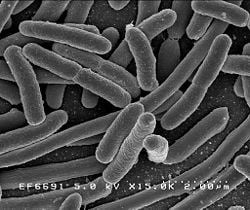
Escherichia coli
| Escherichia coli | ||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|
 | ||||||||||||
|
Conservation status: Secure
| ||||||||||||
| Scientific classification | ||||||||||||
| ||||||||||||
| Escherichia coli T. Escherich, 1885 |
Escherichia coli (IPA: [ˌɛ.ʃəˈɹɪ.kjə ˈkʰoʊ.laɪ]), is one of the well known and significant species of bacteria living as gut fauna in the lower intestines of mammals. The number of individual E. coli bacteria in the feces that a human excretes in one day averages between 100 billion and 10 trillion. For this reason, E. coli has been used in water analysis as the indicator of fecal contamination. However, the bacteria are not confined to this environment, and specimens have also been located, for example, on the edge of hot springs.
E. coli is just one of many microbial species in mammals. For example, the large intestine of humans houses over 700 species of bacteria. These perform a variety of functions, with many benefits for the host organism. For example, bacteria produce enzymes capable of digesting many of the molecules that are indigestible to vertebrates, produce small amounts of vitamins for absorption into the blood, and help to prevent colonization by toxic bacteria. When located in the large intestine, E. coli also provides some of these same values for the host organism, assisting with waste processing, vitamin K production, and food absorption. Remarkably, the human immune system, which is so adept at recognizing invading organisms, does not mobilize against E. coli as a foreign object.
E. coli exists in ever increasing number of strains due to mutation and high frequency recombination (genetic transfer in conjugation). Though people generally understand E. coli as harmless intestinal flora, they are opportunistic and some of the strains have been identified as the serious causal agents of various illness. Furthermore, the health hazards associated with E. coli have become more complicated by the fact that some of the causal agents have developed resistance against usual antibiotics.
Since its discovery in 1885 by Theodor Escherich, a German pediatrician and bacteriologist (Feng et al. 2002), E. coli has been the subject of intense theoretical as well as practical research because of its abundance in close association with human beings. This has surely contributed to better understanding of natural phenomena, especially in the fields of genetics, genetic engineering, and microbiology.
General features
E. coli is a rod shaped, Gram-negative, facultative anaerobe, lactose-fermenting, non–endospore-forming microorganism. Its cell measures 1–2 µm in length and 0.1–0.5 µm in diameter. Its ten flagella are grouped in a peritrical arrangement. Strains of E. coli consist of colicinogeny factor or col plasmid (extra–chromosomal DNA ring), which is responsible for the production of bacteriocin called colicin, a toxin against other strains of the same genus.
E. coli is a member of the family Enterobacteriaceae, which includes many genera, including well known pathogens such as Salmonella, Shigella, and Yersinia. One of the root words of the family's scientific name, "enteric," refers to the intestine, and is often used synonymously with "fecal." All the different kinds of fecal coli bacteria (i.e., E. coli), and all the very similar (twin brother) bacteria that live in the soil or decaying plants (of which the most common is Enterobacter aerogenes), are grouped together under the name coliform. Technically, the "coliform group" is defined to be all the aerobic and facultative anaerobic, non–spore–forming, Gram–negative, rod–shaped bacteria that ferment lactose with the production of gas within 48 hours at 35°C (95°F). In the body, this gas is released as flatulence. Coliform is not a taxonomic classification but rather a working definition.
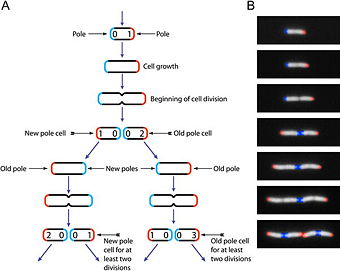
As with other bacteria, E. coli multiplies vegetatively by binary fission. Presence of F factor (fertility factor or sex factor) also has enabled the organism to undergo, here and there, conjugation for lateral DNA transfer between organisms. The F factor is a bacterial DNA sequence that allows a bacterium to produce a sex pilus and a conjugation bridge with another conjugant, necessary for conjugation. It contains 20 tra (for "transfer") genes and a number of other genetic sequences responsible for incompatibility, replication, and other functions. During conjugation in E. coli, genetic material thus may be transferred between the two conjugants and high frequency recombinants (strains with chromosomal DNA of another conjugant being received as an integral part of the plasmid, namely F–factor) may be produced. In addition, genetic transfer also may occur via transduction (transfer of gene via bacteriophage).
E. coli can survive outside of the host for a while, but the disinfection of all active bacteria can be easily carried out by pasteurization or simple boiling, with more rigorous sterilization process not required since the bacteria does not form spores.
Strains
A "strain" of E. coli is a group with some particular characteristics that make it distinguishable from other E. coli groups. These differences are often detectable only on the molecular level; however, they may cause changes in the physiology or life cycle of the bacterium, leading for example to the different level of pathogenicity (ability of an organism to cause disease in another organism).
Different strains of E. coli live in different kinds of animals, so it is possible to trace whether the fecal material in water came from from humans or from birds, for example.
New strains of E. coli arise all the time from the natural biological process of mutation, and some of those strains develop characteristics that can be harmful to their host animal. Although in most healthy adult humans such a strain would probably cause no more than a bout of diarrhea, and might produce no symptoms at all, in young children, people who are or have recently been sick, or in people taking certain medications, such a strain can cause serious illness and even death. The E. coli strain O157:H7 is one of hundreds of strains of the bacterium that is virulent and causes illness in humans (CCID/DBMD 2006).
Since E. coli and related bacteria possess the ability to transfer DNA via bacterial conjugation and bacteriophages, a new mutation can spread more widely through an existing population. It is believed that this process led to the spread of toxin synthesizing capability from Shigella to E. coli O157:H7.
The combination of letters and numbers in the name of the bacterial strain refers to the specific markers found on its surface and distinguishes it from other strains of E. coli. E. coli O157:H7 is said to possess 5,000 genes in its genome, which is around 1,000 genes more than that of other strains (NIH/NIAID 2001).
Extended–Spectrum Beta–Lactamase (ESBL)–producing E. coli are antibiotic–resistant strains. They produce an enzyme called extended–spectrum beta lactamase, which makes them resistant to antibiotics, thus making the infections harder to treat. In many instances, only a few oral antibiotics and a very limited group of intravenous antibiotics remain effective.
Detection of E. coli
Detection of E. coli is the only sure way of diagnosis of associated diseases. Furthermore, by detecting its presence or even enumerating its count, the severity of fecal contamination is evaluated and proper suggestions are issued. Thus, there have been different levels of detection of the organism.
As a result of their adaptation to mammalian intestines, different strains of E. coli grows best in vivo or at the higher temperatures characteristic of such an environment, rather than the cooler temperatures found in soil and other environments. The coliforms are very easily differentiated from others by growing them in lactose–peptone–nutrient medium (e.g., Mac–Conkey broth produced by Merck) at 37°C for 48 hours and checking if they can produce acid and gas. The estimation of the number of the cells per unit is carried out by a statistical, multi–step assay called "Most Probable Number (MPN) method."
For further differentiation of the fecal coli, they are grown in lactose–peptone–eosin–methyl blue (EMB) agar medium. After incubating the medium at 37°C for 48 hours, E. coli develops into blue black colonies with light reflecting metallic shine, whereas Enterobacter forms reddish slimy colonies. For E. coli O157:H7, the stool specimen be tested on sorbitol–MacConkey (SMAC) agar.
To perform the complete differentiation of fecal contaminant (e.g., E. coli) and the non–fecal contaminant (e.g., Enterobacter), a series of biochemical tests are used that are collectively known as IMViC test. In these tests, indol production from tryptophan (indol test), production of strong acid causing red color in methyl red indicator (methyl red test), production of acetoine (Voges–Proskauer test), and use of citrate as the only carbon source (citrate test) are conducted. E. coli shows positive reactions for the first two tests whereas Enterobacter aerogenes for the last two tests.
Causal agent of diseases
Although most strains are harmless, E. coli O157:H7 strain produces a powerful toxin that can cause severe illness. Thus E. coli O157:H7 has become a leading cause of food borne illness (CDC 2006). E. coli can generally cause several intestinal and extra–intestinal infections such as urinary tract infections, meningitis, peritonitis, mastitis, septicemia, and gram–negative pneumonia. If E. coli bacteria escape the intestinal tract through a perforation (a hole or tear, for example from an ulcer, a ruptured appendix, or a surgical error), and enter the abdomen, they usually cause peritonitis that can be fatal without prompt treatment.
Mode of transmission
Cattle are the principal source of E. coli O157 infection, as it can live in the intestines of healthy cattle, deer, goats, and sheep; their manure is also an important source. Therefore, most illness has been associated with eating undercooked, contaminated ground beef. Since toxigenic coli can be resident in animals that are resistant to the toxin, they may be spread through direct contact on farms, at petting zoos, and so forth. However, people have also become ill from eating contaminated salami, bean sprouts, or fresh leafy vegetables, such as lettuce and spinach.
Person–to–person contact in families and child care centers is also a known mode of transmission. People who are infected with E. coli are very contagious. In addition, infection can occur after drinking raw milk and after swimming in or drinking sewage contaminated water or juice.
It has also been shown that the strains of E. coli, specifically O157:H7, can be found in filth flies on cattle farms and in house flies and can be transmitted by them (Szalanski et al. 2004; Alam et al. 2004). They can also be transmitted to and by fruit flies to the wounded fruits and from there to people on consumption (Sela et al. 2005). They may also be spread via airborne particle in some environments (Christie 2002).
Gastrointestinal infections
The enteric E. coli are divided on the basis of virulence properties into enterotoxigenic (ETEC, causative agent of diarrhea in humans, pigs, sheep, goats, cattle, dogs, and horses); enteropathogenic (EPEC, causative agent of diarrhea in humans, rabbits, dogs, cats, and horses); enteroinvasive (EIEC, found only in humans); verotoxigenic (VTEC, found in pigs, cattle, dogs, and cats); enterohaemorrhagic (EHEC, found in humans, cattle, and goats); attacking porcine strains that colonize the gut in a manner similar to human EPEC strains; and enteroaggregative E. coli (EAggEC, found only in humans).
Certain strains of E. coli, such as Escherichia coli O157:H7 and E. coli O104:H21, are toxigenic (some produce a toxin very similar to that seen in dysentery) and can cause food poisoning usually associated with eating cheese and contaminated meat (contaminated during or shortly after slaughter or during storage or display). The usual countermeasure is cooking suspect meat "well done"; the alternative of careful inspection of slaughtering and butchering methods (to make sure that the animal's colon is removed and not punctured) has apparently not been systematically tried.
This particular strain is believed to be associated with the 2006 United States E. coli outbreak linked to fresh spinach. Severity of the illness varies considerably. It can be fatal, particularly to young children, the elderly, or the immunocompromised, but is more often mild.
E. coli can harbor both heat–stable and heat–labile enterotoxins. The latter, termed LT, is highly similar in structure and function to Cholera toxin. It contains one "A" subunit and five "B" subunits arranged into one holotoxin. The B subunits assist in adherence and entry of the toxin into host intestinal cells, where the A subunit is cleaved and prevents cells from absorbing water, causing diarrhea. LT is secreted by the Type 2 secretion pathway (Tauschek et al. 2002).
E. coli possess specific nucleation–precipitation machinery to produce soluble amyloid oglimers and precipitate them as curli, a network of fibers which bind the bacteria to host cells and each other. The importance of E. coli as a source or amyloid is unknown, but amyloid fibers are a component of numerous human disease processes including Alzheimer's (Chapman et al. 2002).
Urinary tract infections (UTI)
Although it is more common in females due to the shorter urinary tract, urinary tract infection is seen in both males and females. It is found in roughly equal proportions in elderly men and women. Since bacteria invariably enter the urinary tract through the urethra, called "Ascending infections," poor toilet habits can predispose to infection. However, other factors are also important (pregnancy in women, prostate enlargement in men) and in many cases the initiating event is unclear. While ascending infections are generally the rule for lower urinary tract infections and cystitis, the same may not necessarily hold for upper urinary tract infections like pyelonephritis, which may be hematogenous in origin. Most cases of lower urinary tract infections in females are benign and do not need exhaustive laboratory work ups. However, UTI in young infants must receive some imaging study, typically a retrograde urethrogram, to ascertain the presence/absence of congenital urinary tract anomalies. Males too must be investigated further.
In some persons, E. coli O:157H:7 is further notorious for causing serious, even life threatening complications like Hemorrhagic Uremic Syndrome (HUS). People with this problem get hemolytic anemia (which is a low red blood cell count), thrombocytopenia (which is a low platelet count), and renal failure (which is kidney damage). About 8 percent of persons whose diarrheal illness is severe enough that they seek medical care develop this complication. In the United States, HUS is the principal cause of acute kidney failure in children, and most cases of HUS are caused by E. coli O157:H7 (CDC 2006).
Treatments of E. coli infections
Antibiotic therapy
Appropriate treatment of E. coli infections depends on the disease and should be guided, whenever possible, by laboratory analysis of the antibiotic susceptibilities of the infecting strain. As Gram–negative organisms, E. coli are resistant to many antibiotics that are effective against Gram–positive organisms. Antibiotics that may be used to treat E. coli infection include (but are not limited to) amoxicillin as well as other semi–synthetic penicillins, many cephalosporins, carbapenems, aztreonam, trimethoprim–sulfamethoxazole, ciprofloxacin, nitrofurantoin, and the aminoglycosides. Not all antibiotics are suitable for every disease caused by E. coli, and the advice of a physician should be sought.
Antibiotic resistance is a growing problem. Some of this is due to overuse of antibiotics in humans, but some of it is probably due to the use of antibiotics as growth promoters in food animals (Johnson et al. 2006). Resistance to beta–lactam antibiotics has become more serious in recent decades as strains producing extended–spectrum beta–lactamases render many, if not all, of the penicillins and cephalosporins ineffective as therapy.
E. coli is a frequent member of multispecies biofilms. Some strains are piliated (with F–plasmid) and capable of accepting and transferring plasmids from and to other bacteria of the same and different species. E. coli often carry multidrug resistant plasmids and under stress readily transfer those plasmids to other species. Thus E. coli and the other member of enterobacteriaceae are important reservoirs of transferable antibiotic resistance (Franiczek et al. 2006).
However, E. coli are extremely sensitive to such antibiotics as streptomycin or gentamycin, so treatment with these antibiotics is usually effective. This could rapidly change, since, as noted above, E. coli rapidly acquires drug resistance (NIH 2001). The American Academy of Science suggests to minimize the use of antibiotics.
Phage therapy
Phage therapy is the use of viruses that specifically target pathogenic bacteria. It has been developed over the last 80 years, primarily in the former Soviet Union, where it was used to prevent diarrhea caused by E. coli, among other things, in the Red Army, and was widely available over the counter.
Vaccine
E. coli vaccines have been under development for many years (Girard et al. 2006). In March of 2006, a vaccine eliciting an immune response against the E. coli O157:H7 O-specific polysaccharide conjugated to recombinant exotoxin A of Pseudomonas aeruginosa (O157–rEPA) was reported to be safe and immunogenic in children two to five years old. It has already been proven safe and immunogenic in adults. A phase III clinical trial to verify the large-scale efficacy of the treatment is planned (Ahmed 2006).
In January 2007, the Canadian bio–pharmaceutical company Bioniche announced it has developed a cattle vaccine that reduces the number of bacteria shed in manure by a factor of 1,000, to about 1,000 bacteria per gram of manure (Pearson 2007; CanadaAM 2007; BionichePR 2007).
Significance in microbiology
Because of its ubiquity, E. coli is frequently studied in microbiology and is commonly used as a model organism for the study of bacteria in general. Its structure has already been clearly understood, and it makes for an excellent target for novice, intermediate, and advanced students of the life sciences. Fertility factor (F–Plasmid) and bacterial conjugation were first discovered in E. coli, and it remains the primary model to study conjugation and gene transfer.
It is the current "workhorse" in molecular biology. The strains used in the laboratory have adapted themselves effectively to that environment, and are no longer as well adapted to life in the mammalian intestines as the wild type. A major adaptation is the loss of the large quantities of external biofilm mucopolysaccharide produced by the wild type in order to protect itself from antibodies and other chemical attacks, but which require a large expenditure of the organism's energy and material resources. This can be seen when culturing the organisms on agar plates; while the laboratory strains produce well defined individual colonies, with the wild type strains the colonies are embedded within this large mass of mucopolysaccharide, making it difficult to isolate individual colonies.
Because of this long history of laboratory culture and manipulation, E. coli plays an important role in modern biological engineering. Researchers can alter the bacteria to serve as "factories" to synthesize DNA and/or proteins, which can then be produced in large quantities using the industrial fermentation processes. One of the first useful applications of recombinant DNA technology was the manipulation of E. coli to produce human insulin for patients with diabetes. Scientists are synthetically engineering E. coli that can target and kill cancer cells (Singer 2006).
Significance in determining water purity and sewage treatment
On the basis of microbiological examination of water, its portability (suitability for drinking) may be ascertained. The presence of coliform bacteria in surface water is a common indicator of fecal contamination.
In the field of water purification and sewage treatment, E. coli was chosen very early in the development of the technology as an "indicator" of the pollution level of water, meaning the amount of human fecal matter in it. E. coli is used for detection because it makes up about 10 percent of intestinal microorganisms of human and animals; consequently, there are a lot more coliforms in human feces than there are pathogens. (Salmonella typhi is an example of such a pathogen, causing typhoid fever). E. coli is usually harmless, so it can't "get loose" in the lab and hurt anyone.
The test for the presence of coliform in water has traditionally involved three routine standard tests: (a) the presumptive test, (b) the confirmed test, and (c) the complete test. The presumptive test just observes for the coliforms in terms of gas production from lactose fermentation. As the gas production occurs not only due to fecal contaminants, but also non–fecal contaminants as well as non–coliforms, those positive presumptive tests are further analyzed by the confirmed test. Here the special feature of fecal coli (E. coli) is tested, like metallic sheen exhibited by the colonies in EMB–agar medium, and so forth. To complete the sanitary test, those positive in the confirmed test are checked for gas production and the morphological features of E. coli.
In addition, the number of coliforms as well as E. coli per unit volume of water sample can be estimated using the MPN (most probable number) tests. Comparing the number of coliform/E. coli with the standardized coliform index, the water quality can be graded and recommended for certain use or none. Many of these tests are routinely done at water storage and distribution systems.
However, sometimes it can be misleading to use E. coli alone as an indicator of human fecal contamination because there are other environments in which E. coli grows well, such as paper mills. At other places, more advanced tests have replaced them. Other organisms like Streptococcus bovis and certain Clostridium species are also used as an index of fecal contamination of drinking water sources.
ReferencesISBN links support NWE through referral fees
- Ahmed, A, J. Li, Y. Shiloach, J. B. Robbins, and S. C. Szu. 2006. Safety and immunogenicity of Escherichia coli O157 O-specific polysaccharide conjugate vaccine in 2-5-year-old children. The Journal of Infectious Diseases 193(4): 515-521. PMID 16425130.
- Alam, M. J. and L. Zurek. 2004. Association of Escherichia coli O157:H7 with houseflies on a cattle farm. Appl Environ Microbiol 70(12): 7578-7580. PMID 15574966.
- Bioniche Life Sciences. 2007. Canadian research collaboration produces world's first food safety vaccine: Against E. coli 0157:H7. Bioniche Life Sciences. Retrieved September 29, 2007.
- CCID/DBMD. 2006. Escherichia coli O157:H7. Department of Health and Human Services, Centers for Disease Control and Prevention, Division of Bacterial and Mycotic Diseases, Coordinating Center for Infectious Diseases. Retrieved September 29, 2007.
- Chapman, M. R., L. S. Robinson, J. S. Pinkner, R. Roth, J. Heuser, M. Hammar, S. Normark, and S. J. Hultgren. 2002. Role of Escherichia coli curli operons in directing amyloid fiber formation. Science 295(5556): 851-855. PMID 11823641.
- Christie, T. 2002. Tests suggest E. coli spread through air. The Register-Guard. Retrieved September 29, 2007.
- CTV. 2007. New cattle vaccine controls E. coli infections. CTV Canada AM. Retrieved September 29, 2007.
- Feng, P., S. Weagant, and M. Grant. 2002. Enumeration of Escherichia coli and the coliform bacteria. Bacteriological Analytical Manual Online. FDA/Center for Food Safety & Applied Nutrition. Retrieved September 29, 2007.
- Franiczek, R., I. Dolna, B. Krzyzanowska, K. Szufnarowski, B. Kowalska-Krochmal, and M. Zielińska. 2006. Conjugative transfer frequency of resistance genes from ESBL-producing Enterobacteriaceae strains isolated from patients hospitalized in pediatric wards. Med Dosw Mikrobiol 58(1): 41-51. PMID 16871972.
- Girard, M. P., D. Steele, C. L. Chaignat, and M. P. Kieny. 2006. A review of vaccine research and development: Human enteric infections. Vaccine 24(15): 2732-2750. PMID 16483695.
- Johnson, J. R., M. A. Kuskowski, M. Menard, A. Gajewski, M. Xercavins, and J. Garau. 2006. Similarity between human and chicken Escherichia coli isolates in relation to ciprofloxacin resistance status. The Journal of Infectious Diseases 194(1): 71-78. PMID 16741884.
- NIH. 2001. Gene sequence of deadly E. coli reveals surprisingly dynamic genome. NIH/National Institute Of Allergy And Infectious Diseases. Science Daily. Retrieved September 29, 2007.
- Pearson, H. 2007. The dark side of E. coli. Nature 445(7123):8-9. PMID 17203031.
- Sela, S., D. Nestel, R. Pinto, E. Nemny-Lavy, and M. Bar-Joseph. 2005. Mediterranean fruit fly as a potential vector of bacterial pathogens. Appl Environ Microbiol 71(7):4052-4056. PMID 16000820.
- Singer, E. 2006. tumor-killing bacteria. Scientists are synthetically engineering E. coli that can target and kill cancer cells. Applied and Environmental Microbiology 66(12): 5155-5160. Retrieved October 22, 2007.
- Szalanski, A. L., C. B. Owens, T. McKay, and C. D. Steelman. 2004. Detection of Campylobacter and Escherichia coli O157:H7 from filth flies by polymerase chain reaction. Med Vet Entomol 18(3): 241-246. PMID 15347391.
- Tauschek, M., R. J. Gorrell, R. A. Strugnell, and R. M. Robins-Browne. 2002. Identification of a protein secretory pathway for the secretion of heat-labile enterotoxin by an enterotoxigenic strain of Escherichia coli. PNAS 99(10): 7066-7071. Retrieved September 29, 2007.
Credits
New World Encyclopedia writers and editors rewrote and completed the Wikipedia article in accordance with New World Encyclopedia standards. This article abides by terms of the Creative Commons CC-by-sa 3.0 License (CC-by-sa), which may be used and disseminated with proper attribution. Credit is due under the terms of this license that can reference both the New World Encyclopedia contributors and the selfless volunteer contributors of the Wikimedia Foundation. To cite this article click here for a list of acceptable citing formats.The history of earlier contributions by wikipedians is accessible to researchers here:
The history of this article since it was imported to New World Encyclopedia:
Note: Some restrictions may apply to use of individual images which are separately licensed.