Prostate
| Prostate | |
|---|---|
| Male Anatomy | |
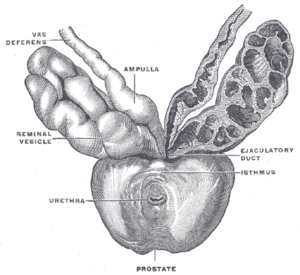
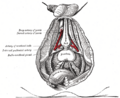
| Prostate with seminal vesicles and seminal ducts, viewed from in front and above. | |
| Latin | prostata |
| Gray's | subject #263 1251 |
| Artery | internal pudendal artery, inferior vesicle artery, and middle rectal artery |
| Vein | internal iliac vein |
| Nerve | inferior hypogastric plexus |
| Lymph | external iliac lymph nodes, internal iliac lymph nodes |
| Precursor | Endodermic evaginations of the urethra |
| MeSH | Prostate |
| Dorlands/Elsevier | p_36/12671161 |
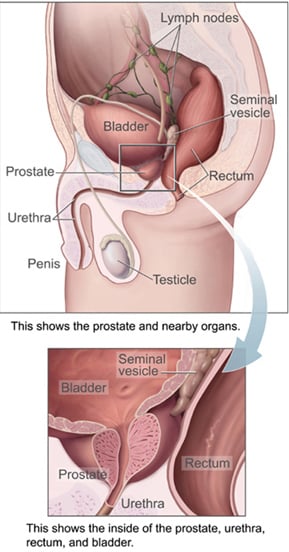
The prostate or prostate gland is a exocrine gland of the male mammalian reproductive system, located at the base of the urinary bladder. It is a compound tubuloalveolar gland (start out as branched tubular, tube-shaped, and branches further to terminate in alveoli). The prostate differs considerably between species anatomically, chemically, and physiologically. It secretes a fluid that is a substantial part of the semen and can regulate urine flow.
In human males, the prostate gland is the size and shape of a chestnut, surrounds the urethra, and consists of 15 to 50 glands that open into the urethra. There is no such gland in females.
The prostate reveals the intricate harmony in the human reproductive process. The alkaline fluid secreted by the prostate is believed to aid in sperm motility. This fluid counters the more acidic fluid from the seminal vesicles and the environment in the female uterus. This intricate coordination between the various elements—urinary bladder, urethra, seminal vesicles, uterus, and so forth, must work in harmony for successful sexual reproduction. Furthermore, harmony is revealed in the process whereby the prostate provides a value to the body, and in turn the body provide the nutrients needed for maintenance of the prostate.
At times, however, this intricate harmony breaks down. Of the several diseases affecting the prostate, the most serious is prostate cancer. Among the many risk factors for prostate cancer that have been identified in epidemiological and environmental studies are exposure to various pollutants and over-consumption of dietary fat (Flatto 1990; Pienta and Esper 1993), as well as promiscuity and sexual hyperactivity (Flatto 1990; MH 2006), with greater risk tied to increased number of sexual partners (Schuman et al. 1977; Steele et al. 1971), extramarital sexual relationships (Steele et al. 1971), and early age at onset of sexual activity (Schuman et al. 1977). Particularly, promiscuity of men in their younger years appears to increase risk of developing prostate cancer (MH 2006; Leake 2004), possibly explaining the rapid increase in incidence of this disease.
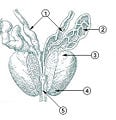
Structure of the human prostate
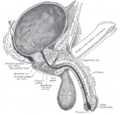
The prostate is located under and in front of the male’s urinary bladder. A healthy human prostate is slightly larger than a walnut and somewhat triangular, being more rounded at the top, with the more pointed apex directed downward and forward.
The prostate surrounds the beginning of the urethra, just below the urinary bladder. The urethra is a tube that connects the male and female’s urinary bladder to the outside of the body. The urethra has an excretory function in both genders to pass urine to the outside, but in males it also serves a reproductive function, as passage for sperm. In males, the urethra runs through the prostate and opens at the end of the penis. In surrounding the urethra, the prostate has two lobes connected anteriority by an isthmus and in the posterior by a middle lobe.
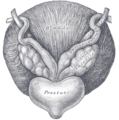
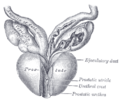
The prostate has several openings that lead into the first part of the urethra, called the prostatic urethra. Two of these are ejaculatory ducts from the seminal vesicles that carry sperm and fluid from the seminal vesicles. The seminal vesicles are located above and behind the prostrate, and the ejaculatory ducts penetrate the prostate gland and enter the urethra within the prostate. In addition, the prostate has numerous, branched, tubular glands (15 to 50) that open into the urethra. These glands are surrounded by connective tissue (stroma). These glands secrete into the urethra a thin, viscid, milky, alkaline fluid that is considered to be important for sperm motility.
The prostate and can be felt during a rectal exam.
The prostate can be divided in two different ways: By zone or by lobe.
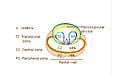
Zones
The "zone" classification is more often used in pathology.
The prostate gland has four distinct glandular regions, two of which arise from different segments of the prostatic urethra:
| Name | Percent | Description |
| The Peripheral Zone (PZ) | Comprises up to 70 percent of the normal prostate gland in young men | The sub-capsular portion of the posterior aspect of the prostate gland, which surrounds the distal urethra. It is from this portion of the gland that more than 70 percent of prostatic cancers originate. |
| The Central Zone (CZ) | Constitutes approximately 25 percent of the normal prostate gland | This zone surrounds the ejaculatory ducts. Central zone tumors account for more than 25 percent of all prostate cancers. |
| The Transition Zone (TZ) | Responsible for 5 percent of the prostate volume | This zone is very rarely associated with carcinoma. The transition zone surrounds the proximal urethra and is the region of the prostate gland that grows throughout life and is responsible for the disease of benign prostatic enlargement. |
| The Anterior Fibro-muscular zone (or stroma) | Accounts for approximately 5 percent of the prostatic weight | This zone is usually devoid of glandular components, and composed only, as its name suggests, of muscle and fibrous tissue. |
Lobes
The "lobe" classification is more often used in gross anatomy.
| anterior lobe (or isthmus) | roughly corresponds to part of Transitional Zone |
| posterior lobe | roughly corresponds to Peripheral Zone |
| lateral lobes | spans all zones |
| median lobe (or middle lobe) | roughly corresponds to part of Central Zone |
Function
The main function of the prostate is to store and secrete a clear, slightly alkaline fluid that constitutes 10-30 percent of the volume of the seminal fluid that, along with spermatozoa, constitutes semen. The rest of the seminal fluid is produced by the two seminal vesicles. The alkaline secretion of the prostate is believed to help sperm motility, and thus, fertilization of an egg, because sperm are more mobile in relatively alkaline medium. This secretion counters the more acidic fluid from the testes and seminal vesicles, and neutralizes the acidity of the vagina.
The prostate also contains some smooth muscles that help expel semen during ejaculation.
Prostatic secretions vary between species. They are generally composed of simple sugars. In human prostatic secretions, the protein content is less than 1 percent and includes proteolytic enzymes, acid phosphatase, and prostate-specific antigen. The secretions also contain zinc and citric acid.
To work properly, the prostate needs male hormone (androgens), which are responsible for male sex characteristics. The main male hormone is testosterone, which is produced mainly by the testicles. Some male hormones are produced in small amounts by the adrenal glands.
Development
The prostate gland represents the modified wall of the proximal portion of the male urethra and develops by the ninth week of embryonic life. Condensation of mesenchyme, urethra, and Wolffian ducts gives rise to the adult prostate gland, a composite organ made up of several glandular and non-glandular components tightly fused within a common capsule.
Skene's glands, found in many females, are homologous to the prostate gland in males.
Prostate disorders
Prostatitis
Prostatitis is inflammation of the prostate gland. There are four basic categories of prostatitis, each with different causes and outcomes. Acute prostatitis (bacterial) and chronic bacterial prostatitis are treated with antibiotics; chronic prostatitis (non-bacterial) or male chronic pelvic pain syndrome, which comprises about 95 percent of prostatitis diagnoses, is treated by a large variety of modalities, including alpha blockers, physical therapy, psychotherapy, antihistamines, anxiolytics, nerve modulators, and more (Theoharides and Sant 2001; CP 2003). The fourth category, asymptomatic inflammatory prostatitis, does not require treatment. Symptoms vary with the category of disease. In acute prostatitis (bacterial), men often experience such symptoms as chills, fever, pain in the lower back and genital area, urinary frequency and urgency often at night, burning or painful urination, body aches, and a demonstrable infection of the urinary tract, as evidenced by white blood cells and bacteria in the urine. There may be discharge from the penis. In chronic prostatitis/chronic pelvic pain syndrome (CP/CPPS), there is pelvic pain of unknown cause, lasting longer than 6 months, as the key symptom. Symptoms may wax and wane. Pain can range from mild discomfort to debilitating. Pain may radiate to back and rectum, making sitting difficult. Dysuria, arthralgia, myalgia, unexplained fatigue, abdominal pain, constant burning pain in the penis, and frequency may all be present. Frequent urination and increased urgency may suggest interstitial cystitis (inflammation centered in bladder rather than prostate). Chronic bacterial prostatitis is a relatively rare condition and is defined as recurrent urinary tract infections in men originating from a chronic infection in the prostate. Symptoms may be completely absent until there is also bladder infection, and the most troublesome problem is usually recurrent cystitis. In asymptomatic inflammatory prostatitis, patients have no history of genitourinary pain complaints, but leukocytosis or bacteria have been noted during evaluation for other conditions
Benign prostatic hyperplasia
Benign prostatic hyperplasia (BPH), also known as nodular hyperplasia, benign prostatic hypertrophy, or benign enlargement of the prostate (BEP), refers to the increase in size of the prostate in middle-aged and elderly men. The prostate often enlarges to the point it may constrict the urethra and impede the flow of urine, making urination difficult and painful, and in extreme cases completely impossible. To be accurate, the process is one of hyperplasia rather than hypertrophy, but the nomenclature is often interchangeable, even amongst urologists. Hyperplasia is a proliferation of cells within an organ or tissue beyond that which is ordinarily seen, due to cell division increasing the number of cells; hypertrophy occurs do to an increase in the size of cells, while the number stays the same.
BPH is characterized by hyperplasia of prostatic stromal and epithelial cells, resulting in the formation of large, fairly discrete nodules in the periurethral region of the prostate. When sufficiently large, the nodules compress the urethral canal to cause partial, or sometimes virtually complete, obstruction of the urethra, which interferes the normal flow of urine. It leads to symptoms of urinary hesitancy, frequent urination, increased risk of urinary tract infections, and urinary retention. Although prostate specific antigen levels may be elevated in these patients, because of increased organ volume and inflammation due to urinary tract infections, BPH is not considered to be a premalignant lesion.
Benign prostatic hyperplasia symptoms are classified as obstructive or irritative. Obstructive symptoms include hesitancy, intermittency, incomplete voiding, weak urinary stream, and straining. Irritative symptoms include frequency of urination, which is called nocturia when occurring at night time, and urgency (compelling need to void that cannot be deferred).
BPH can be treated with medication or with surgery that removes part of the prostate. The surgery most often used in such cases is called transurethral resection of the prostate (TURP or TUR). In TURP, an instrument is inserted through the urethra to remove prostate tissue that is pressing against the upper part of the urethra and restricting the flow of urine. Older men often have corpora amylacea (amyloid), dense accumulations of calcified proteinaceous material in the ducts of their prostates. The corpora amylacea may obstruct the lumens of the prostatic ducts and may underlie some cases of BPH.
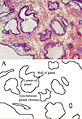
Prostate Cancer
Prostate cancer is one of the most common cancers affecting elderly men in developed countries and a major cause of death. Cancer occurs when cells of the prostate mutate and begin to multiply out of control. These cells may spread (metastasize) from the prostate to other parts of the body, especially the bones and lymph nodes.
Prostate cancer develops most frequently in men over fifty. It is the most common type of cancer in men in the United States, where it is responsible for more male deaths than any other cancer, except lung cancer. However, many men who develop prostate cancer never have symptoms, undergo no therapy, and eventually die of other causes. Many factors, including genetics and diet, have been implicated in the development of prostate cancer.
Regular rectal exams are recommended for older men to detect prostate cancer early. Prostate cancer is most often discovered by physical examination or by screening blood tests, such as the PSA (prostate specific antigen) test. There is some current concern about the accuracy of the PSA test and its usefulness. Suspected prostate cancer is typically confirmed by removing a piece of the prostate (biopsy) and examining it under a microscope. Further tests, such as X-rays and bone scans, may be performed to determine whether prostate cancer has spread.
Prostate cancer can be treated with surgery, radiation therapy, hormone therapy, occasionally chemotherapy, proton therapy, or some combination of these.
Additional images
ReferencesISBN links support NWE through referral fees
- Chronic Prostatis.com. 2003. Pharmacological treatment options for prostatitis/chronic pelvic pain syndrome. Chronic Prostatis.com. Retrieved June 5, 2007.
- Flatto, E. 1990. Coffee drinking and sexual desire—prostate cancer, bicycle riding and sexual interest, vaginal spotting, penile implants, diet and fertility, spontaneous orgasm—The Doctor's Casebook. Nutrition Health Review Fall, 1990. Retrieved June 5, 2007.
- Leake, J. 2004. Promiscuity linked to prostate cancer. Wrong Diagnosis (from the Sunday Times, Britain). Retrieved June 5, 2007.
- Men's Health (MH). 2006. Prostate cancer linked to promiscuity. Menshealth.com. Retrieved June 5, 2007.
- National Kidney and Urologic Diseases Information Clearinghouse, U. S. National Institutes of Health. 2002. What I need to know about prostate problems. NIH Publication No. 02-4806 (a public domain resource). Retrieved June 5, 2007.
- Pienta, K. J., and P. S. Esper. 1993. Risk factors for prostate cancer. Annals of Internal Medicine 118(10): 793-803.
- Schuman, L., M. Mandel, C. Blackard, H. Bauer, J. Scarlett, and R. McHugh. 1977. Epidemiologic study of prostatic cancer: A preliminary report. Cancer Treat Rep 61: 181-186.
- Steele, R., R. E. Lees, A. S. Kraus, and C. Rao. 1971. Sexual factors in the epidemiology of cancer of the prostate. J Chronic Dis 24: 29-37.
- Theoharides, T. C., and G. R. Sant. 2001. New agents for the medical treatment of interstitial cystitis. Exp. Opin. Invest. Drugs 10(3): 521-546.
External links
All links retrieved December 2, 2022.
- "Drug hope in prostate cancer care", from BBC News.
Credits
New World Encyclopedia writers and editors rewrote and completed the Wikipedia article in accordance with New World Encyclopedia standards. This article abides by terms of the Creative Commons CC-by-sa 3.0 License (CC-by-sa), which may be used and disseminated with proper attribution. Credit is due under the terms of this license that can reference both the New World Encyclopedia contributors and the selfless volunteer contributors of the Wikimedia Foundation. To cite this article click here for a list of acceptable citing formats.The history of earlier contributions by wikipedians is accessible to researchers here:
- Prostate history
- Urethra history
- Benign_prostatic_hyperplasia history
- Organ_hypertrophy history
- Prostate_cancer history
The history of this article since it was imported to New World Encyclopedia:
Note: Some restrictions may apply to use of individual images which are separately licensed.