Scabies
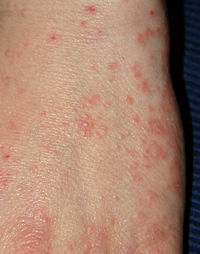
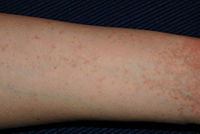
Scabies is a transmissible ectoparasite skin infection caused by tiny mites of the species Sarcoptes scabiei, with the disease characterized by intense itching (pruritus), a rash, and secondary infection, as well as superficial burrows where mites tunnel under the skin of their hosts. The human scabies mite, Sarcoptes scabiei var. hominis, is responsible for human infections. Domestic and wild animals also may be infected by various varieties of Sarcoptes mites, such as S. scabiei var. canis, which is a parasite of dogs and foxes. Varieties affecting domestic animals may be transferred to humans (Chakrabarti 1985; Ulmer et al. 2007; Mumcuoglu and Rufli 1979). This article will be about infection in humans, unless otherwise stated.
Scabies is most prevalent among people in overcrowded conditions and conditions of poor hygiene (Carson-DeWitt 2002). This is a preventable disease and one tied to issues of personal responsibility, including good hygiene. There are readily available treatments for this condition, as well as means to prevent reinfection tied to cleaning of one's environment and personal items, such as clothing. Ultimately, this is a disease that could be significantly reduced, if not exterminated, through individuals taking special precautions to prevent the spread of these mites, which cannot survive long outside of the human skin.
The word scabies comes from the Latin word for "scratch" (scabere).
Overview
In humans, scabies is caused by the tiny mite Sarcoptes scabiei, variety hominis. Scabies was one of the earliest human diseases with a known cause (Arlian 1989). The mite was first described and illustrated in 1689, by the Italians Diancinto Cestoni and Giovanni Cosimo Bonomo in a now-famous letter to Francesco Redi (Arlian 1989). However, only some 200 years later, was it generally accepted that scabies was a parasitic disease (Arlian 1989).
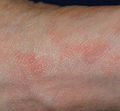
S. scabiei var. hominis infection produces intense, itchy skin rashes when the impregnated female mite tunnels into the skin's outermost layer, the stratum corneum, and deposits eggs in the burrow. Upon hatching, the larvae move to the surface of the skin, molt into a "nymphal" stage, mature into adult mites, and mate, and repeat the life cycle either within the original host or its next host (Carson-DeWitt 2002; Jacques 2008). The action of the mites moving within the skin and on the skin itself produces an intense itch, which may resemble an allergic reaction in appearance. The presence of the eggs produces a massive allergic response which, in turn, produces more itching.
Scabies is transmitted readily, often throughout an entire household, by skin-to-skin contact with an infected person (for example, bed partners, schoolmates, daycare). Spread by clothing, bedding, or towels is a less significant risk, though possible.
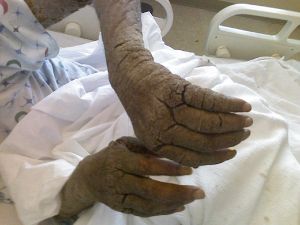
In individuals with strong immune systems and those that scratch (which apparently, often inadvertently, removes some of the mites), infections commonly involve no more than 15 mites altogether, with an average of 11 adult females in an affected human host (Jacques 2008; Carson-DeWitt 2002). However, in those physically infirm, or otherwise immunocompromized, such as the elderly, there may be an infection with a more severe variant called crusted scabies or Norwegian scabies, with a human host infected by thousands to more than two million adult females (Jacques 2008; Carson-DeWitt 2002). This type of infection involves thickened, crusty areas all over the body (Carson-DeWitt 2002).
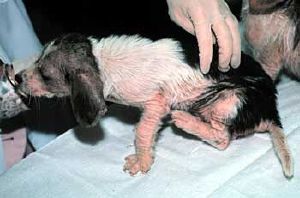
Various varieties of Sarcoptes scabiei may infect wild and domestic animals. S. scabiei var. canis is parasitic on dogs, foxes, and wolves, causing sarcoptic mange, and it can also infect cats and humans to a lesser extent. S. scabiei var. wombati affects wombats. S. scabiei var. cuniculi is the rabbit scabies mite. S. scabiei var. bovis infects cattle.
S. scabiei mites typically are adapted to their preferred host or hosts, and they may be unable to complete their life cycle in other, dissimilar hosts. Nonetheless, often they can transfer to other hosts, including humans, causing opportunistic infections. Mumcuoglu and Rufli (1979) report a case where S. scabiei var. bovis infected a farmer. They further reported that this variety penetrates the human skin, but does not form burrows, which is in contrast to typical S. scabiei infections of preferred hosts, such as with variety hominis affecting humans. S. scabiei var. wombati likewise only burrows in a short way in opportunistic infections of humans.
Sarcoptes scabiei
| Sarcoptes scabiei | ||||||||||||||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
 | ||||||||||||||||||||||||||
| Scientific classification | ||||||||||||||||||||||||||
| ||||||||||||||||||||||||||
| Sarcoptes scabiei De Geer, 1778 |
Sarcoptes scabiei is a tiny mite, a parasitic arthropod (phylum Arthropoda) belonging to the class Arachnida, subclass Acarina (or Acari), a taxon that contains ticks as well, the order astigmata, and the family Sarcoptidae.
As members of the class Arachnida, mites would be expected to have a segmented body with the segments organized into two tagmata: A prosoma (cephalothorax) and an opisthosoma (abdomen). However, only the faintest traces of primary segmentation remain in mites, the prosoma and opisthosoma are insensibly fused, and a region of flexible cuticle (the cirumcapitular furrow) separates the chelicerae and pedipalps from the rest of the body. This anterior body region is called the capitulum or gnathosoma and is also found in the Ricinulei. The remainder of the body is called the idiosoma and is unique to mites.
The sarcoptes are part of the larger family of mites collectively known as “scab mites;” they are also related to the scab mite “psoroptes,” also a mite that infests the skin of domestic animals. Sarcoptic mange affects domestic animals and similar infestations in domestic fowls causes the disease known as “scaly leg.”
S. scabiei is only about 0.3 to 0.4 millimeters (.012 to .016 inches) long as an adult (Jacques 2008; Carson-DeWitt 2002). The type that infects humans is Sarcoptes scabiei, variety hominis. Scabies are microscopic, although sometimes they are visible as a pinpoint of white.
The life cycle of mites includes four stages: Egg, larva, nymph, and adult. The life cycle of Sarcoptes scabiei, variety hominis involves the female burrowing under the lower stratum corneum of the skin and laying eggs in small numbers along the line of the burrow (Arlian 1989; Carson-DeWitt 2002). The six-legged larvae hatch in about three to ten days and move toward the surface of the skin, where they will make new burrows and mature. Specifically, the larvae search for hair follicles, where they feed and molt (discard old cuticles to grow), and mature into adult mites. It is in the hair follicles that the larvae show the first nymphal stage, with eight legs. After reaching maturity and being fertilized, the adult female mite burrows into the skin, of either the same host or a new host, and then lays its eggs, completing the life cycle. The life cycle is about three to four weeks in total (Jacques 2008).
The female has more molts than a male and, therefore, takes longer to reach adulthood—seventeen days for the female versus nine to eleven days for a male. The female is about twice the size of the male. Males tend to roam on top of the skin, although they can and do occasionally burrow. Both males and females surface at times, especially at night.
The action of the mites moving within the skin and on the skin itself produces an intense itch which may resemble an allergic reaction in appearance. The presence of the eggs produces a massive allergic response which, in turn, produces more itching.
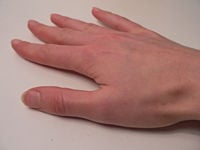
The adult female usually burrows into the hands or wrists; however, other parts of the body may also be affected, and lays its eggs. The burrowing is carried out using the mouthparts and special cutting surfaces on the front legs. While these are being used, Sarcoptes scabiei anchors itself with suckers on its feet.
Although the life cycle is short, individual patients are seldom found to have more than about a dozen mites on them. Even so, this number can cause agonizing itching, in particular at night, and severe damage to the skin often comes as a result of scratching, particularly by the introduction of infective bacteria, which may lead to impetigo or eczema.
The conditions most favorable to Sarcoptes scabiei are found on parts of the human body, such as the hands and wrists, where there is frequent skin to skin contact between persons, as the mites are transmitted by skin contact with carriers, and they very easily spread.
The mites can live away from human skin for only about three days (Carson-DeWitt 2002; CDC 2008).
Signs, symptoms, and diagnosis
Symptoms develop approximately four to six weeks after initial infestation. Therefore, infected persons may have been contagious for at least a month before being diagnosed and may have passed scabies to anyone with whom they had close contact. Persons who sleep in the same room with a person with scabies has a high possibility of having scabies as well, although they may not show symptoms.
The symptoms are caused by an allergic reaction that the body develops over time to the mites and their by-products under the skin, such as the feces; thus the four to six week "incubation" period.
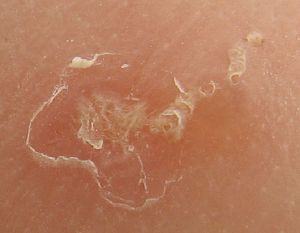
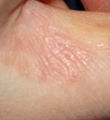
Diagnosis is usually achieved by observing the characteristic burrows of the mites (Carson-DeWitt 2002). A tiny mite may sometimes be seen at the end of a burrow. Burrows are located most commonly on the sides of fingers, between the fingers, on top of the wrists, around the armpits and elbows, around the nipples in women's breasts, in the genitalia of men, around the waist (beltline), and the lower part of the buttocks (Carson-DeWitt 2002). Babies may have burrows on the palms of their hands, soles of their feet, and faces (Carson-DeWitt 2002). The face usually does not become involved in adults.
When a suspected burrow is found, diagnosis may be confirmed by microscopy of surface scrapings. The pearly bump at the end of a burrow can be removed and examined microscopically, possibly identifying the mite itself (Carson-DeWitt 2002). Skin scrapings may be placed on a slide in glycerol, mineral oil, or immersion in oil and covered with a coverslip. Avoiding potassium hydroxide is necessary because it may dissolve fecal pellets. Positive diagnosis is made when the mite, ova, or fecal pellets are found.
Finding burrows may be difficult because they are scarce, or because they are obscured by scratch marks, or by secondary dermatitis (unrelated skin irritation). If burrows are not found in the primary areas known to be affected, the entire skin surface of the body should be examined.
Scabies is frequently misdiagnosed as intense pruritus (itching of healthy skin) before papular eruptions form. Upon initial pruritus, the burrows appear as small, barely noticeable bumps on the hands and may be slightly shiny and dark in color rather than red. Initially, the itching may not exactly correlate to the location of these bumps. As the infestation progresses, these bumps become more red in color.
The suspicious area can be rubbed with ink from a fountain pen or alternately a topical tetracycline solution which will glow under a special light. The surface is then wiped off with an alcohol pad; if the person is infected with scabies, the characteristic zigzag or S pattern of the burrow across the skin will appear.
The rash may become secondarily infected as scratching the rash may break the skin and make such infection more likely.
People with compromised a immune system may develop crusted Norwegian scabies. In this case, they may be infected with huge numbers of mites—thousands or even millions. Examples of cases in which individuals do not scratch (and thus inadvertently remove mites) or have weakened immune systems include: the physically infirm; those where other diseases that decrease the sensation in the skin; those with leukemia or diabetes; those taking medication that lowers the immune response; and those patients with AIDS that have a lower immune response (Carson-DeWitt 2002). Likewise, in people being treated with immunosuppressive drugs like steroids, the elderly, or those mentally handicapped, a widespread rash with thick scaling may result. These cases require additional treatment options to ensure a complete kill. Ivermectin is a single oral treatment of choice in these patients combined with any other topical treatment.
Treatment
Some impact is made simply by the patient scratching or washing. Although not a cure, this helps to keep the total population low. (However scratching should be done with a washcloth to avoid cutting the skin, as this can lead to infection.), Also, humans create antibodies to the scabies mites, which do kill some of them.
Treatment options include various medications.
Medications
Topical
- Permethrin. The topical medication of choice is five percent permethrin because it is safe for all age groups (Scheinfeld 2004).
- Eurax (USP Crotamiton).
- Malathion. Applied for 24 hours is effective in killing adults and eggs.
- Lindane (Kwellada). For use with patients with whom permethrin has failed or is contraindicated (CDER 2003). Lindane is FDA approved as safe and effective when used as directed for the second-line treatment for both scabies and lice. Serious side effects are rare and have almost always resulted from product misuse (CDER 2002). However, it is less commonly used because of the risk of nerve toxicity in children (Jacques 2008).
- Ten percent sulfur ointment. Can be used in pregnant women and infants under two months of age. It is available over-the-counter.
Medications typically are applied from head to foot (avoiding the eyes and mouth) and left on overnight (Jacques 2008).
Oral
A single dose of ivermectin has been reported to cure scabies. In 1999, a small scale test comparing topically applied Lindane to orally administered ivermectin found no statistically-significant differences between the two treatments (AAFP 2000).
Preventing reinfection
All family and close contacts should be treated at the same time, even if asymptomatic. Cleaning of the environment should occur simultaneously, as there is a risk of reinfection. Since the scabies mites can, on average, survive only up to 48-72 hours away from human skin (CDC 2008), shoes or other articles that cannot be washed can be sealed in a plastic bag for week or longer (Jacques 2008). (In cases of Crusted Scabies, mites can survive up to seven days.) Therefore, it is recommended to wash all material (such as clothes, bedding, and towels) that has been in contact with all infested persons in the last three days.
Cleaning the environment should include:
- Vacuuming floors, carpets, and rugs
- Disinfecting floor and bathroom surfaces by mopping
- Cleaning the shower/bath tub after each use
- Daily washing of recently worn clothes, towels, and bedding in hot water and drying in a hot dryer
- Consistently rubbing antibacterial lotion on infected areas
- Trying to keep infected areas covered by clothing or band aids
- Hot drying pillows for 30 minutes
- Overnight freezing, in a plastic bag: Stuffed animals, brushes, combs, shoes, coats, gloves, hats, robes, wetsuits, and so forth.
- Quarantine in a plastic bag for two weeks: Things that cannot be washed, hot dried, frozen, or drycleaned.
- Drycleaning: Things that cannot be washed, hot dried, or frozen or quarantined.
Itchiness during treatment
Options to combat itchiness include antihistamines such as cetirizine. Prescription: Doxepin (Sinequan; oral or Zonalon; topical) or Hydroxine.
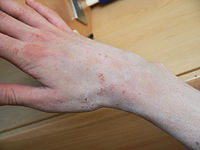
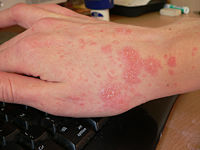
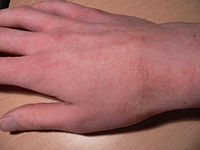
Gallery of scabies infections
ReferencesISBN links support NWE through referral fees
- American Academy of Family Physicians (AAFP). 2000. Efficacy and safety of therapy for human scabies infestation. American Academy of Family Physicians. Retrieved May 17, 2008.
- Arlian, L. G. 1989. Biology, host relations, and epidemiology of Sarcoptes scabiei. Annual Review of Entomology 34: 139-159. Retrieved May 17, 2008.
- Carson-DeWitt, R. 2002. In J. L. Longe (ed.), The Gale Encyclopedia of Medicine, Volume 4, 2nd edition. Detroit: Gale Group/Thomson Learning. ISBN 0787654930.
- Center for Drug Evaluation and Research (CDER). 2003. FDA Public Health Advisory: Safety of topical lindane products for the treatment of scabies and lice. Food and Drug Administration. Retrieved May 17, 2008.
- Center for Drug Evaluation and Research (CDER). 2002. Lindane post marketing safety review. Food and Drug Administration. Retrieved May 17, 2008.
- Centers for Disease Control (CDC). 2008. Scabies. Centers for Disease Control. Retrieved May 17, 2008.
- Chakrabarti, A. 1985. Some epidemiological aspects of animal scabies in human population. Int J Zoonoses 12(1): 39-52. PMID 4055268 Retrieved May 17, 2008.
- Jacques, L. B. 2008. Scabies. In A. Chang, et al. (medical consultants), MaGill's Medical Guide, Volume IV, 4th edition. Pasadena, CA: Salem Press. ISBN 9781587653889.
- Mumcuoglu, Y. and T. Rufli. 1979. Human infestation by Sarcoptes scabiei var. bovis (cattle itch mite). Hautarzt. 30(8):423-6.
- Scheinfeld, N. S. 2004. Controlling scabies in institutional settings: A review of medications, treatment models, and implementation. Amer J Clin Dermatol 5(1): 31-7.
- Ulmer, A., S. Schanz, M. Röcken, and G. Fierlbeck. 2007. A papulovesicular rash in a farmer and his wife. Clin Infect Dis 45(3): 395-96. PMID 17599314
Credits
New World Encyclopedia writers and editors rewrote and completed the Wikipedia article in accordance with New World Encyclopedia standards. This article abides by terms of the Creative Commons CC-by-sa 3.0 License (CC-by-sa), which may be used and disseminated with proper attribution. Credit is due under the terms of this license that can reference both the New World Encyclopedia contributors and the selfless volunteer contributors of the Wikimedia Foundation. To cite this article click here for a list of acceptable citing formats.The history of earlier contributions by wikipedians is accessible to researchers here:
The history of this article since it was imported to New World Encyclopedia:
Note: Some restrictions may apply to use of individual images which are separately licensed.