Acetylcholine

| |
| |
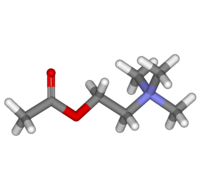
Acetylcholine
| |
| Systematic name | |
| IUPAC name 2-acetoxy-N,N,N-trimethylethanaminium | |
| Identifiers | |
| CAS number | 51-84-3 |
| ATC code | S01EB09 |
| PubChem | 187 |
| DrugBank | EXPT00412 |
| Chemical data | |
| Formula | C7H16NO2 |
| Mol. weight | 146.21 g/mol |
| SMILES | CC(OCC[N+](C)(C)C)=O |
| Pharmacokinetic data | |
| Bioavailability | ? |
| Metabolism | ? |
| Half life | approximately 2 minutes |
| Excretion | ? |
| Therapeutic considerations | |
| Pregnancy cat. | ? |
| Legal status | ? |
| Routes | ? |
Acetylcholine, often abbreviated as ACh, is a small, organic molecule that is a derivative of choline and acetic acid and serves as an important neurotransmitter. Neurotransmitters are chemical compounds that relay information across the gap (synapse) between one neuron (nerve cell) and an adjacent cell (neuron, muscle cell, gland cell). In the case of acetylcholine, it is active both at the synapses between neurons and in the stimulation of muscle cells at the neuromuscular junction. It also stimulates secretion of glands.
As a neurotranmsitter in neuron-to-neuron synapses, acetylcholine is released by the axon terminal end of one neuron, in response to an electrical impulse, and travels across the microscopic synapse in milliseconds to the dendrites of the adjacent neuron, where it is recognized by a receptor site. The neurotransmitter then stimulates a continuation of the electrical impulse in the adjoining neuron.
As a neurotransmitter in neuron to muscle junctions, electrical stimulation of the neuron results in release of acetycholine that can stimulate such muscles as skeletal muscle, smooth muscle, and cardiac tissue. Acetylcholine is both utilized in contraction of skeletal muscle and the slowing of the heart beat.
The synthesis, transport, storage, and action of acetylcholine reveals the remarkable and intricate coordination seen in nature, involving conversion of electrical impulses to chemical transmitters, various enzyme-catalyzed chemical reactions, acetylcholine receptors, calcium ion channels, and sodium channels, removal of the neurotransmitters after they have acted, and so forth.
Discovery of the mechanism of acetylcholine's action and development of applications of that knowledge reflect the diversity of types of outcomes that may result from an original discovery. Knowledge of acetylcholine's role in living systems has been applied toward developing insecticides aimed to improve human life; it has also been applied in developing nerve agents, such as Sarin gas, based on inactivation of a key enzyme in the process.
Acetylcholine was the first neurotransmitter to be identified.
Overview
The transmission of messages over the juncture between a nerve cell and another cell requires that electrical signals be converted to chemical signals. The chemical messenger is termed a neurotransmitter.
Acetylcholine is synthesized in neurons utilizing the enzyme choline acetyltransferase. It is stored at the ending of the neurons in membrane-enclosed vesicles (synaptic vesicles), and released in response to a nerve impulse traveling down the neuron.
Acetylcholine is a neurotransmitter released by neurons in both the peripheral nervous system (PNS) and central nervous system (CNS) in many organisms, including humans (Blakemore and Jennett 2001). The peripheral nervous system (PNS) is that portion of the vertebrate nervous system that is outside the brain and spinal cord, which comprise the central nervous system (CNS). The peripheral nervous system is divided into two subsystems, the somatic nervous system and the autonomic nervous system. The autonomic nervous system is that part of the peripheral nervous system that largely acts independent of conscious control (involuntarily) and consists of nerves in cardiac muscle, smooth muscle, and exocrine and endocrine glands. The somatic nervous system consists of cranial and spinal nerves that innervate skeletal muscle tissue and are more under voluntary control (Anissimov 2006; Towle 1989).
In the autonomic nervous system, acetylcholine serves as a neurotransmitter at both nerve-to-nerve synapses (for both the sympathetic and parasympathetic divisions) and is released at the endings of the parasympathetic nerve fibers on smooth (non-voluntary) muscle, the heart, and glandular cells (Blakemore and Jennett 2001). In the later case, this causes contraction of smooth muscle (such as in the gut), secretion of glands, and slowing of the heart rate and contraction strength.
In the somatic nervous system, acetylcholine acts between motor nerves and the fibers (cells) of skeletal muscle at all neuromuscular junctions (Blakemore and Jennett 2001). The cell membrane of the muscle fiber is close to the release point of the nerve at the motor end plate. The synapse between the nerve and muscle cell is so small that acetylcholine acts almost immediately, starting the series of chemical and physical events that cause contraction of the muscle (Blakemore and Jennett 2001). The action of the acetylcholine is also terminated rapidly, in around 10 milliseconds, largely because of an enzyme (cholinesterase) breaking down the transmitter (Blakemore and Jennett 2001).
In the central nervous system, acetylcholine serves as an important transmitter at nerve-to-nerve synapses in the brain.
Chemistry and overall process
Acetylcholine is an ester of acetic acid and choline, with the chemical formula CH3COOCH2CH2N+(CH3)3. This structure is reflected in the systematic name, 2-acetoxy-N,N,N-trimethylethanaminium.
Acetylcholine (ACh) was first identified in 1914, by Henry Hallett Dale for its actions on heart tissue. It was confirmed as a neurotransmitter by Otto Loewi, who initially gave it the name vagusstoff because it was released from the vagus nerve. Both received the 1936 Nobel Prize in Physiology or Medicine for their work.
Acetylcholine is manufactured in a neuron and transported to the axon terminal, where it is packaged in hundreds of thousands of small, membrane-bound bags called vesicles. When an action potential travels to the synapse, the rapid depolarization causes calcium ion channels to open. Calcium, normally low inside the cell, now enters the nerve ending. Calcium then stimulates the transport of hundreds of vesicles to the synaptic membrane; the vesicles and cell membrane fuse, leading to the release of the packaged neurotransmitters, a mechanism called exocytosis.
The neurotransmitter then diffuses across the synaptic cleft to bind to receptors on adjacent cells.
Later work showed that when acetylcholine binds to acetylcholine receptors on skeletal muscle fibers, it opens ligand gated sodium channels in the membrane. Sodium ions then enter the muscle cell, stimulating muscle contraction. Acetylcholine, while inducing contraction of skeletal muscles, instead induces decreased contraction in cardiac muscle fibers. This distinction is attributed to differences in receptor structure between skeletal and cardiac fibers. Acetylcholine is also used in the brain, where it tends to cause excitatory actions. The glands that receive impulses from the parasympathetic part of the autonomic nervous system are also stimulated in the same way.
Synthesis and degradation
Acetylcholine is synthesized in certain neurons by the enzyme choline acetyltransferase from the compounds choline and acetyl-CoA. Organic mercurial compounds have a high affinity for sulfhydryl groups, which causes dysfunction of the enzyme choline acetyl transferase. This inhibition may lead to acetylcholine deficiency, and can have consequences on motor function.
Normally, the enzyme acetylcholinesterase converts acetylcholine into the inactive metabolites choline and acetate. This enzyme is abundant in the synaptic cleft, and its role in rapidly clearing free acetylcholine from the synapse is essential for proper muscle function. It is a fast enzyme that can rapidly hydrolyze acetylcholine—10,000 molecules of acetylcholine can be hydrolyzed in one second by one molecule of this enzyme.
The devastating effects of organophosphate-containing nerve agents (for example, Sarin gas) are due to their irreversible inactivation of this enzyme. The active components combine with a residue (constituent) of the amino acid serine in the active site of acetylcholinesterase and inhibit the enzyme. The resulting accumulation of acetylcholine causes continuous stimulation of the muscles, glands, and the central nervous system; victims commonly die of suffocation as they cannot contract their diaphragm. Other organophosphates and some carbamates are effective insecticides because they inhibit acetylcholinasterase in insects. On the other hand, since a shortage of acetylcholine in the brain has been associated with Alzheimer's disease, some drugs that inhibit acetylcholinesterase are used in the treatment of that disease.
Release sites
- Acetylcholine is released in the autonomic nervous system:
- pre- and post-ganglionic parasympathetic neurons
- preganglionic sympathetic neurons (and also postganglionic sudomotor neurons, i.e., the ones that control sweating)
Botulin acts by suppressing the release of acetylcholine. The venom from a black widow spider has the reverse effect.
- All preganglionic autonomic fibers including:
- All preganglionic sympathetic fibers
- All preganglionic parasympathetic fibers
- Preganglionic sympathetic fibers to suprarenal medulla, the modified sympathetic ganglion. On stimulation by acetylcholine, it releases adrenaline and noradrenaline.
- All postganglionic parasympathetic fibers
- Some postganglionic sympathetic fibers
- Secretory fibers to sweat glands
- Vasodilator fibers to blood vessels of skeletal muscles
Acetylcholine receptors and pharmacology
There are two main classes of acetylcholine receptors (AChR) in the membranes of cells: Nicotinic acetylcholine receptors (nAChR) and muscarinic acetylcholine receptors (mAChR). They are named for the ligands used to discover the receptors. Nicotine mimics the action of acetylcholine at nicotinic receptors and muscarine (an alkaloid from the mushroom Amanita muscaria) mimics acetylcholine at the muscarinic receptors (Blakemore and Jennett 2001). Skeletal muscle has nicotinic receptors, while muscarinic recpetors are found in smooth muscle, glands, and the heart.
Nicotinic AChRs are ionotropic receptors permeable to sodium, potassium, and chloride ions. They are stimulated by nicotine and acetylcholine and blocked by curare. Most peripheral AChRs are nicotinic, such as those on the heart and blood vessels or at the neuromuscular junction. They are also found in wide distribution through the brain, but in relatively low numbers.
Muscarinic receptors are metabotropic and affect neurons over a longer time frame. They are stimulated by muscarine and acetylcholine, and blocked by atropine. Muscarinic receptors are found in both the central nervous system and the peripheral nervous system, in heart, lungs, upper GI tract, and sweat glands.
Extracts from the plant Amanita muscaria included this compound, and its action on muscarinic AChRs that increased pupil size was used for attractiveness in many European cultures in the past. Now, acetylcholine is sometimes used during cataract surgery to produce rapid constriction of the pupil. It must be administered intraocularly because corneal cholinesterase metabolizes topically administered ACh before it can diffuse into the eye. It is sold by the trade name Miochol-E (CIBA Vision). Similar drugs are used to induce mydriasis (dilation of the pupil) in cardiopulmonary resuscitation and many other situations.
The disease myasthenia gravis, characterized by muscle weakness and fatigue, occurs when the body inappropriately produces antibodies against acetylcholine receptors, and thus inhibits proper acetylcholine signal transmission. Over time, the motor end plate is destroyed. Drugs that competitively inhibit acetylcholinesterase (e.g., neostigmine or physostigmine) are effective in treating this disorder. They allow endogenously released acetylcholine more time to interact with its respective receptor before being inactivated by acetylcholinesterase in the gap junction.
Blocking, hindering, or mimicking the action of acetylcholine has many uses in medicine. Cholinesterase inhibitors, an example of enzyme inhibitors, increase the action of acetylcholine by delaying its degradation; some have been used as nerve agents (Sarin and VX nerve gas) or pesticides (organophosphates and the carbamates). Clinically, they are used to reverse the action of muscle relaxants, to treat myasthenia gravis, and in Alzheimer's disease (rivastigmine, which increases cholinergic activity in the brain).
ACh receptor agonists
Direct acting
- Acetylcholine
- Bethanechol
- Carbachol
- Cevimeline
- Pilocarpine
- Suberylcholine
Indirect acting (reversible)
Reversibly inhibit the enzyme acetylcholinesterase (which breaks down acetylcholine), thereby increasing acetylcholine levels.
- Ambenomium
- Donepezil
- Edrophonium
- Galantamine
- Neostigmine
- Physostigmine
- Pyridostigmine
- Rivastigmine
- Tacrine
- Carbamate Insecticides (Aldicarb)
Indirect acting (irreversible)
Semi-permanently inhibit the enzyme acetylcholinesterase.
- Echothiophate
- Isoflurophate
- Organophosphate Insecticides (Malathion, Parathion, Azinphos Methyl, Chlorpyrifos, among others)
Reactivation of acetylcholine esterase
- Pralidoxime
ACh receptor antagonists
Antimuscarinic agents
- Atropine
- Ipratropium
- Scopolamine
- Tiotropium
Ganglionic blockers
- Mecamylamine
- Hexamethonium
- Nicotine (in high doses)
- Trimethaphan
Neuromuscular blockers
- Atracurium
- Cisatracurium
- Doxacurium
- Metocurine
- Mivacurium
- Pancuronium
- Rocuronium
- Succinylcholine
- Tubovurarine
- Vecuronium
Uncategorized
- Surugatoxin
- Organophosphates block the breakdown of acetylcholine. Tetrachlorvinphos and other organophosphates operate by blocking acetylcholinesterase, which is an enzyme that breaks down acetylcholine.
ReferencesISBN links support NWE through referral fees
- Anissimov, M. 2007. How does the nervous system work?. Conjecture Corporation: Wise Geek. Retrieved May 13, 2007.
- Blakemore, C. and S. Jennett. 2001. The Oxford Companion to the Body. New York: Oxford University Press. ISBN 019852403X
- Brenner, G. M. and C. W. Stevens. 2006. Pharmacology, 2nd Edition. Philadelphia: W.B. Saunders Company (Elsevier). ISBN 1416029842
- Canadian Pharmacists Association. 2000. Compendium of Pharmaceuticals and Specialties, 25th ed. Toronto: Webcom. ISBN 0919115764
- Carlson, N.R. 2001. Physiology of Behavior, 7th ed. Needham Heights, MA: Allyn and Bacon. ISBN 0205308406
- Gershon, M. D. 1998. The Second Brain. New York: HarperCollins. ISBN 0060182520
- Hasselmo, M. E. 1995. Neuromodulation and cortical function: Modeling the physiological basis of behavior. Behav. Brain Res. 67: 1-27. Retrieved June 23, 2007.
- Towle, A. 1989. Modern Biology. Austin, TX: Holt, Rinehart and Winston. ISBN 0030139198
- Yu, A. J. and P. Dayan. 2005. Uncertainty, neuromodulation, and attention. Neuron 46: 681-692. Retrieved June 23, 2007.
External links
All links retrieved June 14, 2023.
- Acetylcholine Chemistry Explained.
Credits
New World Encyclopedia writers and editors rewrote and completed the Wikipedia article in accordance with New World Encyclopedia standards. This article abides by terms of the Creative Commons CC-by-sa 3.0 License (CC-by-sa), which may be used and disseminated with proper attribution. Credit is due under the terms of this license that can reference both the New World Encyclopedia contributors and the selfless volunteer contributors of the Wikimedia Foundation. To cite this article click here for a list of acceptable citing formats.The history of earlier contributions by wikipedians is accessible to researchers here:
The history of this article since it was imported to New World Encyclopedia:
Note: Some restrictions may apply to use of individual images which are separately licensed.