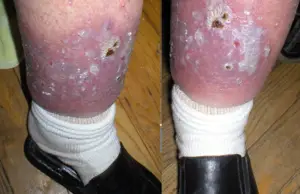
Ulcer
An ulcer (from Latin ulcus) is a lesion or eroded area on the surface of the skin or mucous membranes characterized by tissue disintegration and formation of pus. Essentially, it impacts the epithelium—the tissue that covers organs and surfaces of the bodies of animals, including both outside surfaces (the skin) and inside cavities. As such, an ulcer can impact such areas as the oral cavity and the gastrointestinal tract, the lower extremities, feet, the eyes (most often the cornea), and so forth. However, in common usage, ulcer often is used to refer to peptic ulcers, which are disorders in the part of the digestive tract that includes the stomach, proximal duodenum (and sometimes jejunum) in the small intestine, and the lower part of esophagus.
Causes of ulcers are varied and include injury, circulatory problems (failure of blood supply), infectious agents (bacteria, virus), diseases (typhoid, tuberculosis, bacillary dysentery, syphilis, leprosy, cancer), nutritional deficiencies, burns or other trauma, and so forth. Peptic ulcers, once attributed to stress are now commonly linked to infection by the bacterium Helicobacter pylori, as well as use to use of nonsteroidal anti-inflammatory drugs (NSAIDS, such as aspirin, ibuprofen, etc.), overproduction of digestive juices (Zollinger-Ellison syndrome), among others. Mouth ulcers are often tied to bacterial or viral infections.
In a certain sense, many ulcers are preventable. For example, Longe (2006) lists the use of NSAIDS (nonsteroidal anti-inflammatory drugs, such as aspirin and ibuprofen) as the single most common cause of gastric ulcers. These drugs, which can be obtained without prescription, often are overused, as people look to treat symptoms of headaches, sore muscles, and other complaints without addressing the underlying causes of the complaints. Ulcers of genitalia are most often due to sexually transmitted diseases. Some ulcers are tied to nutritional deficiencies (such as thiamine) and ulcers of the lower extremities are often caused by circulatory problems, some of which may be tied to high cholesterol levels; these two issues are impacted by diet. Such causes reflect the importance of personal responsibility for one's health and perhaps the need for dietary or lifestyle changes.
Description
Ulcers are healing wounds that develop on the skin, mucous membranes, or eye. Although they have many causes, they are marked by:
- Loss of integrity of the area
- Secondary infection of the site by bacteria, fungus, or virus
- Generalized weakness of the patient
- Delayed healing
Essentially, there is disintegration of the tissue (death of cells and tissue), which opens up to the tissue below. The surrounding tissue becomes inflamed. There can also be complications, such as hemorrhage, perforation, and penetration. About five percent of peptic ulcer patients develop perforations: holes in the duodenal or gastric wall through which the contents can leak out into the abdominal cavity (Longe 2006). Penetration involves the ulcer eroding through the intestinal wall without digestive fluid leaking into the abdomen, but rather penetrating into an adjoining organ (Longe 2006).
Pathology of ulceration
Causes
The most common causes (not in order) are:
- Bacterial infection
- Viral infection
- Fungal infection
- Cancer - both 'primary' and 'secondary'
- Venous stasis
- Arterial Insufficiency
- Diabetes
- Rheumatoid Arthritis
- Amyloidosis
- Loss of mobility
- Hypertension
- GERD
- NSAIDS
Longe (2006) reports that the single most common cause of gastric ulcers is the use of nonsteroidal anti-inflammatory drugs, or NSAIDS (aspirin, ibuprofen such as in Advil or Motrin, flubiprofen such as in Ansaid and Ocufen, ketoprofen such as in Orudis, and indomethacin, such as in Indacin). Aspirin is the one most likely to cause ulcers. The causes of duodenal ulcers are most commonly infection with the rod-shaped, gram-negative bacterium Helicobacter pylori (Longe 2006).
Types
Some specific types of ulcers are:
- Peptic ulcer (of the stomach, esophageal cardium, duodenum, or jejunum)
- Mouth ulcer
- Pressure ulcer (decubitus, such as bedsore or pressure sore)
- Crural ulcer (due to venous insufficiency or other causes)
- Hunner's ulcer (of the bladder caused by Interstitial Cystitis)
- Ulcerative colitis (of the colon)
- Curling's ulcer
- Cushing ulcer
- Arterial insufficiency ulcer
- Venous insufficiency ulcer
- Diabetic foot ulcer
- Corneal ulcer
Peptic ulcers include those that develop in the lower part of the esophagus, the stomach, the first part of the small intestine (duodenum), and the middle part of the small intestine) (jejunum) (Longe 2006). The most common peptic ulcers are gastric ulcers (in the stomach) and duodenal ulcers, with about 80 percent of all ulcers in the digestive tract being duodenal ulcers, and 16 percent being peptic ulcers (Longe 2006).
Ulcer classification schemes
The following classification systems are used to communicate the severity and depth of an ulcer. It is an easy way to communicate changes for the better, or worse. The first two are not specific to the location.
Merck Manual classification
- Stage 1: The skin is red. The underlying tissue is soft. The redness disappears with minor pressure.
- Stage 2: There is redness, swelling, and hardening of the skin around the area. Sometimes there is blistering. Sometimes there is loss of the superficial skin.
- Stage 3: The skin becomes necrotic (death of cells and living tissues). There may be exposure of the fat beneath the skin. The skin may be lost through all its layers.
- Stage 4: There is more loss of fat and more necrosis of the skin through to the muscle beneath.
- Stage 5: Continuing loss of fat and necrosis of muscle below.
- Stage 6: Bone destruction begins with irritation of the bone, erosion of the bone cortex progressing to osteomyelitis. There may be sepsis of a joint, pathologic fracture or generalized body infection, septicemia.
National Pressure Ulcer Advisory Panel (NPUAP)
This staging system for rating ulcers is designed to rate the severity of pressure ulcers.
- Stage 1 - There is erythema of intact skin, which does not blanch with pressure. It may be the heralding lesion of skin ulceration.
- Stage 2 - There is partial skin loss involving the epidermis, dermis, or both. The ulcer is superficial and presents as an abrasion, blister, or wound with a shallow center.
- Stage 3 - This is an entire thickness skin loss. It may involve damage to or necrosis of subcutaneous tissue that may extend down to, but not through, the underlying fascia. The ulcer presents as a deep crater with or without undermining of adjacent intact tissues.
- Stage 4 - Here there is entire thickness skin loss with extensive destruction, tissue necrosis, or damage to muscle, bone, or supporting structures. Tendons, and joints may also be exposed or involved. There may be undermining and/or sinus tracts associated with ulcers at this stage.
Wagner's classification
This classification system is intended to rate the severity of diabetic foot ulcerations.
- Grade 0 - Skin with prior healed ulcer scars, areas of pressure that are sometimes called pre-ulcerative lesion, or the presence of bony deformity ,which puts pressure on an unguarded point.
- Grade 1-A - The wound is superficial in nature, with partial or full-thickness skin involvement but does not include tendon, capsule, or bone.
- Grade 1-B - As above, the wound is superficial in nature, with partial or full thickness skin involvement but not including tendon, capsule nor bone; however the wound is infected. The definition of this wound implies superficial infection without involvement of underlying structures. If the wound shows signs of significant purulence or fluctuance, further exploration to expose a higher grade classification of infection is in order.
- Grade 1-C - As above but with vascular compromise.
- Grade 1-D - As above but with ischemia. Because ischemia is a type of vascular compromise, the distinction between these two grades is often difficult to make.
- Grade 2-A - Penetration through the subcutaneous tissue exposing tendon or ligament, but not bone.
- Grade 2-B - Penetration through the deep tissues including tendon or ligament and even joint capsule but not bone.
- Grade 2-C - As above 2B, but including ischemia.
- Grade 2-D - As above 2C, but including infection.
- Grade 3-A - A wound which probes to bone but shows no signs of local infection nor systemic infection.
- Grade 3-B - A wound which probes to bone and is infected.
- Grade 3-C - A wound which probes to bone is infected and is ischemic.
- Grade 3-D - A wound which probes to bone characterized by active infection, ischemic tissues and exposed bone.
- Grade 4 - Gangrene of the forefoot.
- Grade 5 - Gangrene of the entire foot.
ReferencesISBN links support NWE through referral fees
- Blakemore, C., and S. Jennett. 2001. The Oxford Companion to the Body. New York: Oxford University Press. ISBN 019852403X.
- Halpern, G. M. 2004. Ulcer Free!: Nature's Safe & Effective Remedy for Ulcers. Garden City Park, N.Y.: Square One Publishers. ISBN 0757002536.
- Longe, J. L. 2006. The Gale Encyclopedia of Medicine. Detroit: Thomson Gale. ISBN 1414403682.
Credits
New World Encyclopedia writers and editors rewrote and completed the Wikipedia article in accordance with New World Encyclopedia standards. This article abides by terms of the Creative Commons CC-by-sa 3.0 License (CC-by-sa), which may be used and disseminated with proper attribution. Credit is due under the terms of this license that can reference both the New World Encyclopedia contributors and the selfless volunteer contributors of the Wikimedia Foundation. To cite this article click here for a list of acceptable citing formats.The history of earlier contributions by wikipedians is accessible to researchers here:
The history of this article since it was imported to New World Encyclopedia:
Note: Some restrictions may apply to use of individual images which are separately licensed.