Botulinum toxin
| |
Botulinum toxin
| |
| Systematic name | |
| IUPAC name ? | |
| Identifiers | |
| CAS number | 93384-43-1 |
| ATC code | M03AX01 |
| PubChem | ? |
| DrugBank | BTD00092 |
| Chemical data | |
| Formula | C6760H10447N1743O2010S32 |
| Mol. weight | 149320.83328 g/mol |
| Pharmacokinetic data | |
| Bioavailability | ? |
| Metabolism | ? |
| Half life | ? |
| Excretion | ? |
| Therapeutic considerations | |
| Pregnancy cat. | ? |
| Legal status | ? |
| Routes | IM (approved),SC, intradermal, into glands |
Botulinum toxin is any of several distinct types of a neurotoxin protein produced by the bacterium Clostridium botulinum. Botulinum toxin is one of the most poisonous naturally occurring substances in the world, and the most toxic protein known (Montecucco and Molgó 2005).
Though it is highly toxic to humans and can cause botulism, botulinum toxin also is used medicinally in minute doses to block excessive and inappropriate muscle contractions and other therapeutic applications as well as cosmetically, such as to smooth facial lines and wrinkles (McClain 2002).
Botulinum toxin is sold commercially under such brand names Botox, Dysport, and Myobloc for cosmetic purpose. The terms Botox, Dysport, and Myobloc are trade names and are not used generically to describe the neurotoxins produced by C. botulinum.
Source: Clostridium botulinum
Clostridium botulinum is a Gram-positive, rod-shaped bacterium that produces the neurotoxin botulin (botulinum toxin). It is an obligate anaerobe, meaning that oxygen is poisonous to the cells. However, they tolerate very small traces of oxygen due to an enzyme called superoxide dismutase (SOD) which is an important antioxidant defense in nearly all cells exposed to oxygen. Under unfavorable circumstances, they are able to form endospores that allow them to survive in a dormant state until exposed to conditions that can support their growth (Beuchat and Doyle 2007).
Chemical overview and lethality
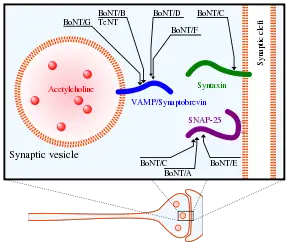
Botulinum toxin, or botulin, is a two-chain polypeptide with a 100-kDa heavy chain joined by a disulfide bond to a 50-kDa light chain. This light chain is an enzyme (a protease) that attacks one of the fusion proteins (SNAP-25, syntaxin or synaptobrevin) at a neuromuscular junction, preventing vesicles from anchoring to the membrane to release acetylcholine. By inhibiting acetylcholine release, the toxin interferes with nerve impulses and causes flaccid (sagging) paralysis of muscles as seen in botulism, as opposite to the spastic paralysis seen in tetanus.
There are seven serologically distinct toxin types, designated A through G. Three subtypes of A have been described. Botulinum toxin type A (BTA-A) and botulinium toxin type B (BTX-B) are use medicinally and cosmetically under various trade names.
Botulinum toxin is possibly the most acutely toxic substance known, with a median lethal dose of about 1 nanogram per kilogram (ng/kg) (Arnon et al. 2001), meaning that a few hundred grams could theoretically kill every human on earth. (For perspective, the rat poison strychnine, often described as highly toxic, has an LD50 of 1,000,000 ng/kg, and would thus take about six metric tons to kill every human.)
Botulinum toxin is also remarkably easy to come by: Clostridium spores are found in soil practically all over the earth.
Food-borne botulism usually results from ingestion of food that has become contaminated with spores (such as a perforated can) in an anaerobic environment, allowing the spores to germinate and grow. The growing (vegetative) bacteria produce toxin. It is the ingestion of preformed toxin that causes botulism, not ingestion of the spores or vegetative organism.
Infant (intestinal) and wound botulism both result from infection with spores that subsequently germinate, resulting in production of toxin and the symptoms of botulism.
The toxin itself is rapidly destroyed by heat, such as in thorough cooking (Licciardello et al. 1967). However, the spores that produce the toxin are heat-tolerant and will survive boiling at 100 degrees Celsius for an extended period of time (Setlowa 2007).
Biochemical mechanism of toxicity
The heavy chain of the botulinum toxin is particularly important for targeting the toxin to specific types of axon terminals of neurons. In order to cause paralysis, the toxin must get inside the axon terminals. Following the attachment of the toxin heavy chain to proteins on the surface of axon terminals, the toxin can be taken into neurons by endocytosis.
The light chain is able to leave endocytotic vesicles and reach the cytoplasm. (Endocytotic vesicles are those membrane-bound vesicles formed by the cell during the process of endocytosis in order to bring extracellular material into the cell. Normally, material remains in the vesicle until degraded by lysosomes.) The light chain of the toxin has protease activity. The type A toxin proteolytically degrades the SNAP-25 protein, a type of SNARE protein. The SNAP-25 protein is required for the release of neurotransmitters from the axon endings (Foran et al. 2003). Botulinum toxin specifically cleaves these SNAREs and so prevents neuro-secretory vesicles from docking/fusing with the nerve synapse plasma membrane and releasing their neurotransmitters.
Though it affects the nervous system, common nerve agent treatments (namely the injection of atropine and 2-pam-chloride) will increase mortality by enhancing botulin toxin's mechanism of toxicity. Attacks involving botulinum toxin are distinguishable from those involving nerve agent in that NBC detection equipment (such as M-8 paper or the ICAM) will not indicate a "positive" when a sample of the agent is tested. Furthermore, botulism symptoms develop relatively slowly, over several days compared to nerve agent effects, which can be instantaneous.
Medical and cosmetic uses
Botulin toxin injections are used therapeutically in very small quantities in conditions of inappropriate and excessive muscle contractions, eye-movement disorders, tics and tremors, sphincter contractions, and spasticity (or muscular hypertonicity, a disorder in which certain muscles are continuously contracted) (McClain 2002). Other medicinal uses of botulin include cervical dystonia or spasmodic torticollis (a neuromuscular disorder involving the head and neck) (Brin et al. 1999), blepharospasm (involuntary blinking) (Shukla and Sharma 2005), severe primary axillary hyperhidrosis (excessive sweating) in palms and armpits (Eisenach et al. 2005; McClain 2002), and achalasia (failure of the lower esophageal sphincter to relax).
Botulin toxin also is used cosmetically to treat facial wrinkles and lines, and is being explored for potential treatment of chronic muscle tension and migraines (McClain 2002). Other uses of botulinum toxin type A that are widely known but not specifically approved by FDA include treatment of pediatric incontinence (Schurch and Corcos 2005), incontinence due to overactive bladder (Duthie et al. 2007), incontinence due to neurogenic bladder (Akbar et al. 2007), anal fissure (Trzciński et al. 2002), and spastic disorders associated with injury or disease of the central nervous system including trauma, stroke, multiple sclerosis, Parkinson's disease, and cerebral palsy.
Treatment and prevention of chronic headache (Panicker and Muthane 2003) and chronic musculoskeletal pain (Charles 2004) are emerging uses for botulinum toxin type A. In addition, there is evidence that botulinum toxin may aid in weight loss by increasing the gastric emptying time (Coskun et al. 2005).
Type A botulinum toxin has an approximately three-month effect on the muscles (McClain 2002). About ninety percent of injections for facial spasms are successful (McClain 2002).
In 2002, approximately 1.1 to 1.6 million patients were using Botulinum toxin type A (BTA) cosmetically (Coté et al. 2005).
Brand names
Botulinum toxin type A (BTA-A) is manufactured as Botox by Allergan (United States) for both therapeutic as well as cosmetic use. Dysport is a therapeutic formulation of the type A toxin developed and manufactured in Ireland and that is licensed for the treatment of focal dystonias and certain cosmetic uses in many territories world wide. Neuronox is a new type A toxin manufactured by Medy-Tox Inc (South Korea).
Trade names for Botulinium toxin type B (BTX-B) are Myobloc in the United States and Neurobloc in the European Union.
Side effects
Bolulinum toxin has been used therapeutically for about thirty years on humans and "has proved to be remarkably safe" (McClain 2002). However, there are difficulties, such as different patients experiencing different effects at similar doses, new patients experiencing exaggerated effects at subsequent treatments, or neighboring muscles impacted (McClain 2002). Generally, multiple injections show a lower incidence of complications versus administration by one larger dose (McClain 2002).
Side effects of botulinum toxin can be predicted from the mode of action (muscle paralysis) and chemical structure (protein) of the molecule, resulting broadly speaking in two major areas of side effects: paralysis of the wrong muscle group and allergic reaction. In cosmetic use, this means that the client will complain of inappropriate facial expression such as drooping eyelid, uneven smile, and loss of ability to close the eye. This will wear off in around 6 weeks. When injecting the masseter muscle of the jaw, loss of muscle function will result in a loss or reduction of power to chew solid foods. All cosmetic treatments are of limited duration, and can be as short a period as six weeks, but an effective period of between three and eight months may be reckoned. At the extremely low doses used medicinally, botulinum toxin has a very low degree of toxicity.
Reported adverse events from cosmetic use includes headaches, focal facial paralysis, muscle weakness, dysphagia, flu-like syndromes, and allergic reactions. Resistance to the toxin is assumed to be the result of circulating antibodies to the toxin (McClain 2002). Those who experience reactions to botulinum toxin may find more success with one of the other serotypes (McClain 2002).
Bruising at the site of injection is a side effect not of the toxin, but rather the mode of administration. Bruising is prevented by the clinician applying pressure to the injection site, but may still occur, and will last around seven to ten days.
Links to deaths
The United States Food and Drug Administration reported that the use of Botox resulted in 28 deaths between 1989 and 2003, though none were attributed to cosmetic use (Coté 2005).
On February 8, 2008, the FDA announced that Botox has "been linked in some cases to adverse reactions, including respiratory failure and death, following treatment of a variety of conditions using a wide range of doses," due to its ability to spread to areas distant to the site of the injection (FDA 2008).
Treatment of botulinum poisoning
The case fatality rate for botulinum poisoning between 1950 and 1996 was 15.5 percent, down from approximately 60 percent over the previous 50 years (CDC 1998). Death is generally secondary to respiratory failure due to paralysis of the respiratory muscles, so treatment consists of antitoxin administration and artificial ventilation. If initiated on time, these are quite effective. Occasionally, functional recovery may take several weeks to months.
There are two primary botulinum antitoxins available for treatment of botulism.
- Trivalent (A,B,E) Botulinum Antitoxin is derived from equine sources utilizing whole antibodies (Fab & Fc portions). This antitoxin is available from the local health department via the Centers for Disease Control (CDC).
- The second antitoxin is Heptavalent (A,B,C,D,E,F,G) Botulinum Antitoxin which is derived from "despeciated" equine IgG antibodies that have had the Fc portion cleaved off leaving the F(ab')2 portions. This is a less immunogenic antitoxin that is effective against all known strains of botulism where not contraindicated. This is available from the U.S. Army.
History
Between 1817 and 1822, the German physician and poet Justinus Kerner described botulinium toxin, using the terms "sausage poison" and "fatty poison" (Erbguth 2004), as this bacterium often causes poisoning by growing in badly handled or prepared meat products. He first conceived a possible therapeutic use of botulinium toxin. In 1870, Müller (another German physician) coined the name botulism, from Latin botulus for "sausage." In 1895, Emile van Ermengem first isolated the bacterium Clostridium botulinum. In 1944, Edward Schantz cultured Clostridium botulinum and isolated the toxin, and, in 1949, Burgen's group discovered that botulinum toxin blocks neuromuscular transmission.
The first medicinal use of botulinum toxin was to treat strabismus (crossed eyes, when the eyes are not properly aligned with each other) (McClain 2002). Alan Scott of the Smith-Kettlewell Institute, who has used botulinium toxin type A (BTX-A) in monkey experiments in 1973, used tiny doses of Botulinum toxin type A for the first time therapeutically in humans, in 1980, to treat strabismus. He also used it as well to treat "uncontrollable blinking" (blepharospasm). Allergan, Inc., a pharmaceutical company that focused on prescription eye therapies and contact lens products, bought the rights to the drug in 1988. Allergan renamed the drug Botox.
Cosmetically desirable effects of Botox were discovered as a result of treating patients for facial spasms and the patients reporting smoothing of facial lines (McClain 2002).
In December 1989, Botulinum toxin type A (BTA-A) (Botox) was approved by the United States Food and Drug Administration (FDA) for the therapeutic treatment of strabismus, blepharospasm, and hemifacial spasm in patients over 12 years old. Botulinium Toxin Type B (BTX-B) received FDA approval for treatment of cervical dystonia on December 21, 2000.
On April 15, 2002, the FDA announced the approval of botulinum toxin type A (Botox Cosmetic) to temporarily improve the appearance of moderate-to-severe frown lines between the eyebrows (glabellar lines). BTX-A has also been approved for the treatment of excessive underarm sweating. The acceptance of BTX-A use for the treatment of spasticity and muscle pain disorders is growing, with approvals pending in many European countries and studies on its use for headaches (including migraine), prostatic symptoms, asthma, obesity, and many other possible indications are ongoing.
ReferencesISBN links support NWE through referral fees
- Akbar, M., R. Abel, T.M. Seyler, H.J. Gerner, and K. Möhring. 2007. Repeated botulinum-A toxin injections in the treatment of myelodysplastic children and patients with spinal cord injuries with neurogenic bladder dysfunction. BJU Int. 100(3): 639–645. Retrieved August 10, 2008.
- Arnon, S.S., R. Schechter, T.V. Inglesby, et al. 2001. Botulinum toxin as a biological weapon: Medical and public health management. JAMA 285(8): 1059-1070. Retrieved August 10, 2008.
- Beuchat, L.R., and M.P. Doyle. 2007. Food Microbiology: Fundamentals and Frontiers. Washington, D.C.: ASM Press. ISBN 9781555814076.
- Brin, M.F., M.F. Lew, C.H. Adler, C.L. Comella, S.A. Factor, J. Jankovic, C. O'Brien, J.J. Murray, J.D. Wallace, A. Willmer-Hulme, and M. Koller. 1999. Safety and efficacy of NeuroBloc (botulinum toxin type B) in type A-resistant cervical dystonia. Neurology 53(7): 1431–8. Retrieved August 10, 2008.
- Centers for Disease Control and Prevention (CDC). 1998. Botulism in the United States, 1899-1996. Handbook for epdemiologgists, clinicians, and laboratory workers. Centers for Diseases Control and Prevention, National Center for Infectious Diseases, Division of Bacterial and Mycotic Diseases. Retrieved August 10, 2008.
- Charles, P.D., 2004. Botulinum neurotoxin serotype A: A clinical update on non-cosmetic uses. American Journal of Health-system Pharmacy 61(22, suppl 6): S11–23. Retrieved August 10, 2008.
- Coskun, H., Y. Duran, E. Dilege, M. Mihmanli, H. Seymen, and M.O. Demirkol. 2005. Effect on gastric emptying and weight reduction of botulinum toxin-A injection into the gastric antral layer: An experimental study in the obese rat model. Obesity Surgery 15(8): 1137–43. Retrieved August 10, 2008.
- Coté, T.R., A. K. Mohan, J.A. Polder, M.K. Walton, and M.M. Braun. 2005. Botulinum toxin type A injections: Adverse events reported to the U.S. Food and Drug Administration in therapeutic and cosmetic cases. J. Am. Acad. Dermatol. 53(3): 407–15. Retrieved August 10, 2008.
- Duthie, J., D. Wilson, G. Herbison, and D. Wilson. 2007. Botulinum toxin injections for adults with overactive bladder syndrome. Cochrane Database Syst Rev. 18;(3):CD005493. Retrieved August 10, 2008.
- Eisenach, J.H., J.L. Atkinson, and R.D. Fealey. 2005. Hyperhidrosis: Evolving therapies for a well-established phenomenon. Mayo Clin. Proc. 80(5): 657–66. Retrieved August 10, 2008.
- Erbguth, F.J. 2004. Historical notes on botulism, Clostridium botulinum, botulinum toxin, and the idea of the therapeutic use of the toxin. Movement Disorders 19(S8): S2–S6. Retrieved August 10, 2008.
- Food and Drug Administration (FDA). 2008. FDA notifies public of adverse reactions linked to Botox use. FDA News. February 8, 2008.
- Foran, P.G., N. Mohammed, G.O. Lisk, et al. 2003. Evaluation of the therapeutic usefulness of botulinum neurotoxin B, C1, E, and F compared with the long lasting type A. Basis for distinct durations of inhibition of exocytosis in central neurons. J. Biol. Chem. 278(2): 1363–71. Retrieved August 10, 2008.
- Licciardello, J.J., J.T. Nickerson, C.A. Ribich, and S.A. Goldblith. 1967. Thermal inactivation of type E botulinum toxin. Appl Microbiol 15(2): 249–56. Retrieved August 10, 2008.
- McClain, B. 2002. Botulinum toxin injections. In J.L. Longe (ed.). The Gale Encyclopedia of Medicine, 2nd edition, volume 1. Detroit: Gale Group/Thomson Learning. ISBN 0787654906.
- Montecucco, C., and J. Molgó. 2005. Botulinal neurotoxins: Revival of an old killer. Current Opinion in Pharmacology 5(3): 274–9. Retrieved August 10, 2008.
- Panicker, J.N., and U.B. Muthane. 2003. Botulinum toxins: Pharmacology and its current therapeutic evidence for use. Neurology India 51(4): 455–60. Retrieved August 10, 2008.
- Schurch, B., and J. Corcos. 2005. Botulinum toxin injections for paediatric incontinence. Current Opinion in Urology 15(4): 264–7. Retrieved August 10, 2008.
- Setlowa, P. 2007. I will survive: DNA protection in bacterial spores. Trends in Microbiology 15 (4): 172–180. Retrieved August 10, 2008.
- Shukla, H.D., and S.K. Sharma. 2005. Clostridium botulinum: A bug with beauty and weapon. Crit. Rev. Microbiol. 31(1): 11–8. Retrieved August 10, 2008.
- Trzciński, R., A. Dziki, and M. Tchórzewski. 2002. Injections of botulinum A toxin for the treatment of anal fissures. European Journal of Surgery 168(12): 720–3. Retrieved August 10, 2008.
Credits
New World Encyclopedia writers and editors rewrote and completed the Wikipedia article in accordance with New World Encyclopedia standards. This article abides by terms of the Creative Commons CC-by-sa 3.0 License (CC-by-sa), which may be used and disseminated with proper attribution. Credit is due under the terms of this license that can reference both the New World Encyclopedia contributors and the selfless volunteer contributors of the Wikimedia Foundation. To cite this article click here for a list of acceptable citing formats.The history of earlier contributions by wikipedians is accessible to researchers here:
The history of this article since it was imported to New World Encyclopedia:
Note: Some restrictions may apply to use of individual images which are separately licensed.