Bleeding
| Bleeding Classification and external resources | |
| ICD-9 | 456.20 |
|---|---|
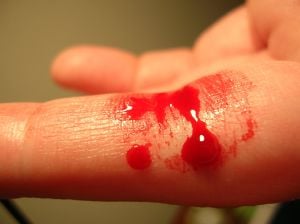
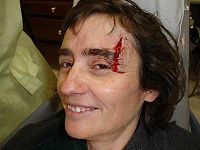
Bleeding is the discharge of blood from blood vessels (arteries, veins, capillaries), whether the blood escapes into internal tissues or outside the body. Hemorrhaging (haemorrhaging in British English) is the technical term for an excessive bleeding in a short period of time whereby the loss of blood might threaten the health or life of the animal or person.
Bleeding can have a wide variety of causes, including trauma or underlying medical conditions. Coagulation disorders are those diseases that involve an inability of the body to control blood clotting, such as hemophilia or thrombocytopenia (Norris 2004). Among other diseases that can result in bleeding are peptic ulcers, scurvy, and hemorrhoids.
The body has a remarkable ability to repair itself in cases of light bleeding, involving a complex and intricately coordinated process known as coagulation. And in some cases, bleeding is perfectly normal, such as for part of the menstrual cycle. However, severe hemorrhaging or bleeding in locations such as the cerebral artery (cerebral hemorrhage), can overwhelm the body's normal protective processes and be debilitating or life-threatening.
Overview
Bleeding involves the escape of blood from blood vessels. A blood vessel is any of the tubular channels that convey blood throughout the body, whether arteries (including threadlike arterioles) that convey blood away from the heart, veins (including threadlike venules) that convey blood toward the heart, or the tiny capillaries that connect arterioles and venules. In vertebrates, blood vessels are part of a complex circulatory system centered on the heart.
When the blood vessels are damaged, bleeding can occur. Such loss of blood can occur internally, where blood leaks from blood vessels inside the body or externally, either through a natural opening such as the vagina, mouth, or anus, or through a break in the skin. The complete loss of blood is referred to as exsanguination, and desanguination is a massive blood loss. In humans, loss of tne to 15 percent of total blood volume can be endured without clinical sequelae in a healthy person. Blood donation, which is not considered to be hemorrhaging because it is done by design, typically takes eight to ten percent of the donor's blood volume (NBS).
When there is bleeding, a complex process known as coagulation, or clotting, works to close the opening by which the blood is escaping. Proteins, coagulation factors, and platelets in the blood plasma result in contraction of the damaged blood vessels so less blood is lost and helps to plug the damaged blood vessels.
Traumas such as a puncture wound can result in rupture of blood vessels and bleeding. Chronic diseases such as atherosclerosis also can affect the walls of blood vessels and result in bleeding. Toxins or septicema (the body's inflammatory response to microbial invaders) cause blood loss through affecting the walls of blood vessels as well. And coagulation disorders, such as hemophilia and low platelet count (thrombocytopenia), affect the body's ability to clot. These may increase the risk of bleeding or may allow otherwise minor bleeds to become health or life threatening. Anticoagulant medications such as warfarin can mimic the effects of hemophilia, preventing clotting and allowing free blood flow.
A slow blood loss can lead to anemia, a qualitative or quantitative deficiency of hemoglobin. A large loss of blood can send the body into shock, a serious, life-threatening medical condition where insufficient blood flow reaches the body tissues. A cerebral hemorrhage (or intracerebral hemorrhage, ICH), is a type of bleeding that occurs within the brain tissue itself and has a high mortality rate.
Hemorrhage generally becomes dangerous, or even fatal, when it causes hypovolemia (low blood volume) or hypotension (low blood pressure). In these scenarios various mechanisms come into play to maintain the body's homeostasis. These include the "retro-stress-relaxation" mechanism of cardiac muscle, the baroreceptor reflex and renal and endocrine responses such as the renin-angiotensin-aldosterone system (RAAS).
Death from hemorrhage can generally occur surprisingly quickly. This is because of 'positive feedback'. An example of this is 'cardiac repression', when poor heart contraction depletes blood flow to the heart, causing even poorer heart contraction. This kind of effect causes death to occur more quickly than expected.
Bleeding has been used as a medical treatment. Before the advent of modern medicine, the technique of bloodletting, or phlebotomy, was used for a number of conditions: causing bleeding intentionally to remove a controlled amount of excess or "bad" blood. Phlebotomy is still used as an extremely effective treatment for hemochromatosis.
Classes of bleeding
Hemorrhaging is broken down into four classes by the American College of Surgeons' Advanced Trauma Life Support (ATLS) (Manning 2004).
- Class I Hemorrhage involves up to 15 percent of blood volume. There is typically no change in vital signs and fluid resuscitation is not usually necessary.
- Class II Hemorrhage involves 15 to 30 percent of total blood volume. A patient is often tachycardic (rapid heart beat) with a narrowing of the difference between the systolic and diastolic blood pressures. The body attempts to compensate with peripheral vasoconstriction. Skin may start to look pale and be cool to the touch. The patient might start acting differently. Volume resuscitation with crystaloids (Saline solution or Lactated Ringer's solution) is all that is typically required. Blood transfusion is not typically required.
- Class III Hemorrhage involves loss of 30 to 40 percent of circulating blood volume. The patient's blood pressure drops, the heart rate increases, peripheral perfusion, such as capillary refill worsens, and the mental status worsens. Fluid resuscitation with crystaloid and blood transfusion are usually necessary.
- Class IV Hemorrhage involves loss of greater than 40 percent of circulating blood volume. The limit of the body's compensation is reached and aggressive resuscitation is required to prevent death.
Individuals in excellent physical and cardiovascular shape may have more effective compensatory mechanisms before experiencing cardiovascular collapse. These patients may look deceptively stable, with minimal derangements in vital signs, while having poor peripheral perfusion (shock). Elderly patients or those with chronic medical conditions may have less tolerance to blood loss, less ability to compensate, and may take medications such as betablockers that can potentially blunt the cardiovascular response. Care must be taken in the assessment of these patients.
The World Health Organization (WHO) also has a standardized grading scale to measure the severity of bleeding:
Grade 0 no bleeding Grade 1 petechial bleeding; Grade 2 mild blood loss (clinically significant); Grade 3 gross blood loss, requires transfusion (severe); Grade 4 debilitating blood loss, retinal or cerebral associated with fatality
Causes of bleeding
Causes of bleeding can be placed into two major categories: trauma and underlying medical conditions.
Traumatic
Traumatic bleeding is caused by some type of injury. There are different types of wounds that may cause traumatic bleeding. These include:
- Abrasion. Also called a graze, this is caused by transverse action of a foreign object against the skin, and usually does not penetrate below the epidermis.
- Excoriation. In common with abrasion, this is caused by mechanical destruction of the skin, although it usually has an underlying medical cause.
- Hematoma. Also called a blood tumor, it is caused by damage to a blood vessel that in turn causes blood to collect under the skin.
- Laceration. This is an irregular wound caused by blunt impact to soft tissue overlying hard tissue or tearing, such as in childbirth. In some instances, this can also be used to describe an incision.
- Incision. This is a cut into a body tissue or organ, such as by a scalpel, made during surgery.
- Puncture wound. A puncture wound is caused by an object that penetrated the skin and underlying layers, such as a nail, needle, or knife.
- Contusion. Also known as a bruise, this is a blunt trauma damaging tissue under the surface of the skin.
- Crushing injury. Crushing injuries are caused by a great or extreme amount of force applied over a long period of time. The extent of a crushing injury may not immediately present itself.
- Gunshot wounds. Caused by a projectile weapon, this may include two external wounds (entry and exit) and a contiguous wound between the two
The pattern of injury, evaluation, and treatment will vary with the mechanism of the injury. Blunt trauma causes injury via a shock effect, delivering energy over an area. Wounds are often not straight and unbroken skin may hide significant injury. Penetrating trauma follows the course of the injurious device. As the energy is applied in a more focused fashion, it requires less energy to cause significant injury. Any body organ (anatomy), including bone and brain, can be injured and bleed. Bleeding may not be readily apparent; internal organs such as the liver, kidney, and spleen may bleed into the abdominal cavity. Bleeding from a bodily orifice, such as the rectum, nose, ears may signal internal bleeding, but cannot be relied upon. Bleeding from a medical procedure also falls into this category.
Due to underlying medical conditions
Medical bleeding is that associated with an increased risk of bleeding due to an underlying medical condition. It may be due to a chronic or acute disease that affects the cell wall (such as aneurysm or septicemia), or coagulation disorders (such as hemophilia A, hemophilia B, or thrombocytopenia).
There are many chronic or acute medical conditions that can affect the cell wall and lead to bleeding. Among these are atherosclerosis (a chronic inflammatory response in the walls of arteries, in large part due to the deposition of lipoproteins); aneurysm (a localized, blood-filled dilation, or balloon-like bulge, of a blood vessel); septicemia (inflammatory state caused by infection, such as microbes in the blood); peptic ulcer (an ulcer of the area of the gastrointestinal tract that is usually acidic and includes the lower part of the esophagus, the stomach, and the duodenum); scurvy (disease resulting from insufficient intake of vitamin C; hemorrhoids (varicosities or swelling and inflammation of veins in the rectum and anus); tuberculosis (infectious disease caused by mycobacteria); and toxins.
Coagulation disorders are those conditions that involve disruption of the body's ability to clot, whether due to an impact on platelet production or one of the many steps in the complex process of coagulation (Norris 2004). Platelets are small blood components that form a plug in the blood vessel wall that stops bleeding. Platelets also produce a variety of substances that stimulate the production of a blood clot. There are several named coagulation factors that interact in a complex way to form blood clots. For instance, deficiency of Factor VIII causes classic Hemophilia A while deficiencies of Factor IX cause "Christmas disease" (hemophilia B). Antibodies to Factor VIII can also inactivate the Factor VII and precipitate bleeding that is very difficult to control. This is a rare condition that is most likely to occur in older patients and in those with autoimmune diseases. Von Willebrand disease is another common bleeding disorder. It is caused by a deficiency of or abnormal function of the "von Willebrand" factor, which is involved in platelet activation. Deficiencies in other factors, such as factor XIII or factor VII are occasionally seen, but may not be associated with severe bleeding and are not as commonly diagnosed. Norris (2004) notes as among the most important coagulation disorders the following:
- Hemophilia A. A genetic disorder that impairs the body's ability to control blood clotting or coagulation due to absence of clotting factor VIII.
- Christmas disease or hemophilia B. A hereditary condition involving a deficiency in clotting factor IX.
- Disseminated intravascular coagulation. A malfunction of clotting factors that causes platelets to clot in small blood vessels and thus there is a lack of clotting factors or platelets at site of injury requiring them.
- Thrombocytopenia. A defective or decreased production of platelets.
- Hypoprothrombinemia. A deficiency in prothrombin, or Factor II.
- Hemophilia C. A deficiency in factor XI.
Leukemia also affects blood coagulation. Leukemia is a cancer of the blood or bone marrow and is characterized by an abnormal proliferation (production by multiplication) of blood cells, usually white blood cells. Damage to the bone marrow, by way of displacing the normal bone marrow cells with higher numbers of immature white blood cells, results in a lack of blood platelets, which are important in the blood clotting process. This means people with leukemia may become bruised, bleed excessively, or develop pinprick bleeds (petechiae).
One of the most common causes of increased bleeding risk is exposure to non-steroidal anti-inflammatory drugs (or "NSAIDs"). The prototype for these drugs is aspirin, which inhibits the production of thromboxane. NSAIDs inhibit the activation of platelets, and thereby increase the risk of bleeding. The effect of aspirin is irreversible; therefore, the inhibitory effect of aspirin is present until the platelets have been replaced (about ten days). Other NSAIDs, such as "ibuprofen" (Motrin) and related drugs, are reversible and therefore, the effect on platelets is not as long-lived.
In addition to NSAID-related bleeding, another common cause of bleeding is that related to the medication, warfarin ("Coumadin" and others). This medication needs to be closely monitored as the bleeding risk can be markedly increased by interactions with other medications. Warfarin acts by inhibiting the production of Vitamin K in the gut. Vitamin K is required for the production of the clotting factors, II, VII, IX, and X in the liver. One of the most common causes of warfarin-related bleeding is taking antibiotics. The gut bacteria make vitamin K and are killed by antibiotics. This decreases vitamin K levels and therefore the production of these clotting factors.
Deficiencies of platelet function may require platelet transfusion while deficiencies of clotting factors may require transfusion of either fresh frozen plasma of specific clotting factors, such as Factor VIII for patients with hemophilia.
First aid
All people who have been injured should receive a thorough assessment. It should be divided into a primary and secondary survey and performed in a stepwise fashion, ideally following the "ABCs." Notification of EMS or other rescue agencies should be performed in a timely manner and as the situation requires.
The primary survey examines and verifies that the patient's Airway is intact, that he or she is Breathing, and that Circulation is working. A similar scheme and mnemonic is used as in CPR. However, during the pulse check of C, attempts should also be made to control bleeding and to assess perfusion, usually by checking capillary refill. Additionally a persons mental status should be assessed (Disability) or either an AVPU scale or via a formal Glasgow Coma Scale. In all but the most minor or obvious cases, the patient should be Exposed by removal of clothing and a secondary survey performed, examining the patient from head to toe for other injuries. The survey should not delay treatment and transport, especially if a non-correctable problem is identified.
Minor bleeding
Minor bleeding is bleeding that falls under a Class I hemorrhage and the bleeding is easily stopped with pressure.
The largest danger in a minor wound is infection. Bleeding can be stopped with direct pressure and elevation, and the wound should be washed well with soap and water. A dressing, typically made of gauze, should be applied. Peroxide or iodine solutions (such as Betadine) can injure the cells that promote healing and may actually impair proper wound healing and delay closure (Wilson et al. 2005).
Emergency bleeding control
Severe bleeding poses a very real risk of death to the casualty if not treated quickly. Therefore, preventing major bleeding should take priority over other conditions, save failure of the heart or lungs. Most protocols advise the use of direct pressure, rest, and elevation of the wound above the heart to control bleeding.
The use of a tourniquet is not advised in most cases, as it can lead to unnecessary necrosis or even loss of a limb.
Bleeding from body cavities
The only minor situation is a spontaneous nosebleed, or a nosebleed caused by a slight trauma (such as a child putting his finger in his nose).
Simultaneous externalized bleeding from the ear may indicate brain trauma if there has been a serious head injury. Loss of consciousness, amnesia, or fall from a height increases the likelihood that there has been a severe injury. This type of injury can also be found in motor vehicle accidents associated with death or severe injury to other passengers.
Hemoptysis, or coughing up blood, may be a sign that the person is at risk for serious bleeding. This is especially the case for patients with cancer. Hematemesis is vomiting up blood from the stomach. Often, the source of bleeding is difficult to distinguish and usually requires detailed assessment by an emergency physician.
Internal bleeding
Internal bleeding occurs entirely within the confines of the body and can be caused by a medical condition (such as aortic aneurysm) or by trauma. Symptoms of internal bleeding include pale, clammy skin, an increased heart rate, and a stupor or confused state.
The most recognizable form of internal bleeding is the contusion or bruise.
Risk of blood contamination
Because skin is watertight, there is no immediate risk of infection to the person providing aid from contact with blood, provided the exposed area has not been previously wounded or diseased. Before any further activity (especially eating, drinking, touching the eyes, the mouth or the nose), the skin should be thoroughly cleaned in order to avoid cross contamination.
To avoid any risk, the hands can be prevented from contact with a glove (mostly latex or nitrile rubber), or an improvised method such as a plastic bag or a cloth. This is taught as important part of protecting the rescuer in most first aid protocols.
Following contact with blood, some rescuers may choose to go to the emergency department, where post-exposure prophylaxis can be started to prevent blood-borne infection.
ReferencesISBN links support NWE through referral fees
- Healthline. n.d. Bleeding Healthline. Retrieved August 31, 2008.
- Manning, J. E. 2004. Fluid and blood resuscitation. In J. E. Tintinalli, G. D. Kelen, and J. S. Stapczynski, eds., Emergency Medicine: A Comprehensive Study Guide. New York: McGraw-Hill. ISBN 0071388753.
- National Blood Service (NBS) for England & North Wales. n.d. Blood donation information UK National Blood Service. Retrieved August 31, 2008.
- Norris, T. 2004. Coagulation disorders. Pages 826-830 in J. L. Longe, The Gale Encyclopedia of Medicine, 2nd edition, volume 2. Detroit, MI: Gale Group/Thomson Learning. ISBN 0787654914 (volume); ISBN 0787654892 (set).
- Webert, K. E., R. J. Cook, C. S. Sigouin, et al. 2006. The risk of bleeding in thrombocytopenic patients with acute myeloid leukemia. Haematologica 91:1530-1537
- Wilson, J. R., J. G. Mills, I. D. Prather, and S. D. Dimitrijevich. 2005. A toxicity index of skin and wound cleansers used on in vitro fibroblasts and keratinocytes Adv Skin Wound Care 18(7):373-8. PMID 16160464.
Credits
New World Encyclopedia writers and editors rewrote and completed the Wikipedia article in accordance with New World Encyclopedia standards. This article abides by terms of the Creative Commons CC-by-sa 3.0 License (CC-by-sa), which may be used and disseminated with proper attribution. Credit is due under the terms of this license that can reference both the New World Encyclopedia contributors and the selfless volunteer contributors of the Wikimedia Foundation. To cite this article click here for a list of acceptable citing formats.The history of earlier contributions by wikipedians is accessible to researchers here:
The history of this article since it was imported to New World Encyclopedia:
Note: Some restrictions may apply to use of individual images which are separately licensed.