Peptic ulcer
| ICD-10 | K25-26 |
|---|---|
| ICD-O: | {{{ICDO}}} |
| ICD-9 | 531-534 |
| OMIM | {{{OMIM}}} |
| MedlinePlus | {{{MedlinePlus}}} |
| eMedicine | {{{eMedicineSubj}}}/{{{eMedicineTopic}}} |
| DiseasesDB | {{{DiseasesDB}}} |
A peptic ulcer is an ulcer of the area of the gastrointestinal tract that is usually acidic and includes the lower part of the esophagus, the stomach, and the duodenum (first part of the small intestine). Some also include the jejunum (second part of the small intestine) (Longe 2006). This condition also is known as peptic ulcer disease or PUD. "Peptic" refers to the enzyme pepsin, a digestive protease in the stomach that digests food proteins into peptides.
An ulcer is a lesion or eroded area on the surface of the skin or mucous membranes characterized by tissue disintegration. Essentially, it impacts the epithelium—the tissue that covers organs and surfaces of the bodies of animals, including both outside surfaces (the skin) and inside cavities. As such, an ulcer can impact such areas as the the oral cavity, the lower extremities, feet, the eyes (most often the cornea), and so forth. However, in common usage, ulcer often is used to refer to peptic ulcers, which are disorders in the upper digestive tract.
The most common peptic ulcers are gastric ulcers, which occur in the stomach, and duodenal ulcers, which occur in the first part of the small intestine (duodenum). About 80 percent of all ulcers in the digestive tract are duodenal ulcers, and about 16 percent of peptic ulcers are gastric ulcers (Longe 2005).
Ulcers in general have a variety of causes, including injury, circulatory problems, infectious agents, disease, trauma, and so forth. While stress and diet were commonly attributed as causes of peptic ulcers, peptic ulcers are now linked primarily to infection by the bacterium Helicobacter pylori, as well as use to use of nonsteroidal anti-inflammatory drugs (NSAIDS, such as aspirin, ibuprofen, etc.), and in some cases overproduction of digestive juices (Zollinger-Ellison syndrome), among others.
The discovery that H. pylori infection is a major cause of peptic ulcers is a triumph of two researchers, Robin Warren and Barry Marshall, who had the courage to speak out over the prevailing scientific dogma. They were able to keep an open mind and see what others had seen; but think what others had not thought (Van der Weyden et al. 2005). It also reflects the commitment of the discoverers: When the hypothesis was poorly received, Marshall successfully infected himself with the bacterium in support for their novel concept.
Longe (2006) lists the use of NSAIDS as the single most common cause of gastric ulcers. These drugs, which can be obtained without prescription, often are overused, as people look to treat symptoms of headaches, sore muscles, and other complaints without addressing the underlying causes of the complaints. Such causes reflect the importance of personal responsibility for one's health and perhaps the need for dietary or lifestyle changes.
Types
Peptic ulcers are the most common ulcers of the gastrointestinal tract. A peptic ulcer may arise at various locations:
- Stomach (called gastric ulcer)
- Duodenum (called duodenal ulcer)
- Esophagus (called esophageal ulcer)
- A Meckel's diverticulum
Longe (2006) also recognizes peptic ulcers as occurring in the jejunum, the portion of the small intestine after the duodenum.
Contrary to general belief, more peptic ulcers arise in the duodenum (first part of the small intestine, just after the stomach) than in the stomach.
About two percent of the population in the United States are estimated to have active peptic ulcers, and ten percent will develop such ulcers during their lifetime (Longe 2006). The male female ratio is 3:1 (Longe 2006). Duodenal ulcers occur in all age groups but are most common between the age of 20 and 45; gastric ulcers are most common between the age of 55 and 70 (Longe 2006). While the incidences of duodenal ulcers in the United States has been declining, incidences of gastric ulcers in rising (Longe 2006).
Causes
The linings in the gastrointestinal tract normally can resist the digestive acids produced. Ulcers develop when this protective ability is reduced and the lining breaks down.
The most common causes of peptic ulcers are bacterial infection, NSAIDS (nonsteroidal anti-inflammatory drugs), and disorders that cause oversecretion of digestive juices.
- Helicobacter pylori infection. A major causative factor is chronic inflammation due to Helicobacter pylori, a rod-shaped, gram-negative bacteria that colonizes the mucous tissues (the antral mucosa) in the digestive tract. The immune system is unable to clear the infection, despite the appearance of antibodies. Thus, the bacterium can cause a chronic active gastritis (type B gastritis), resulting in a defect in the regulation of gastrin production by that part of the stomach, and gastrin secretion is increased. Gastrin, in turn, stimulates the production of gastric acid by parietal cells. The acid erodes the mucosa and causes the ulcer. This bacterium is the most common cause of duodenal ulcers, being considered the causal factor in about 90 percent of the cases. In Western countries, the prevalence of Helicobacter pylori infections roughly matches age (i.e., 20 percent at age 20, 30 percent at age 30, 80 percent at age 80, etc.). Prevalence is higher in Third World countries. Transmission is by food, contaminated groundwater, and through human saliva (such as from kissing or sharing food utensils.) A minority of cases of Helicobacter infection will eventually lead to an ulcer and a larger proportion of people will get non-specific discomfort, abdominal pain, or gastritis.
- NSAIDS. Another major cause of peptic ulcers is the use of NSAIDs, a group of painkillers that includes aspirin, ibuprofen (Advil, Motrin), ketoprofen ( Orudis), flubiprofen (Ansaid, Ocufen), and indomethacin (Indocin) (Longe 2006). The gastric mucosa protects itself from gastric acid with a layer of mucous, the secretion of which is stimulated by certain prostaglandins. NSAIDs block the function of cyclooxygenase 1 (cox-1), which is essential for the production of these prostaglandins. Longe (2006) reports that the single most common cause of gastric ulcers is the use of NSAIDS, and that aspirin is the one most likely to cause ulcers. (Other reports place Helicobacter pylori as the primary cause in gastric ulcers.) Newer NSAIDs (celecoxib, rofecoxib) only inhibit cox-2, which is less essential in the gastric mucosa, and roughly halve the risk of NSAID-related gastric ulceration.
- Other causes. After Helicobacter pylori and NSAIDS, there are other causes that account for the remaining about five percent of ulcers. One is Zollinger-Ellison syndrome in which small tumors secrete the hormone gastrin stimulates the production of digestive acids (Longe 2006). About four percent of stomach ulcers are caused by a malignant tumor, so multiple biopsies are needed to make sure. (Duodenal ulcers are generally benign.)
Other notable factors considered
- Stress. For nearly 100 years, scientists and doctors thought that peptic ulcers were caused by stress (as well as spicy food and alcohol). Treatment involved bed rest and a bland diet. With the discovery that bacterial infection is the cause of most peptic ulcers, it is now common to dismiss stress as a causal agent. However, there remains some debate as to whether stress in a psychological sense can influence the development of peptic ulcers. There is some evidence that stress triggers some ulcers and impairs response to treatment, and some feel that the presence of Helicobacter pylori infection remains inadequate as a monocausal explanation given that this bacterium appears in the gastrointestinal tract of many people that do not develop ulcers. An expert panel convened by the Academy of Behavioral Medicine Research concluded that ulcers are not purely an infectious disease and that psychological factors do play a significant role (SWO 1998). A study of peptic ulcer patients in a Thai hospital showed that chronic stress was strongly associated with an increased risk of peptic ulcer, and a combination of chronic stress and irregular mealtimes was a significant risk factor (Wachirawat 2003). One research avenue is the possibility that psychological stress functions as a cofactor with H. pylori. For example, this bacterium thrives in an acidic environment, and stress has been demonstrated to cause the production of excess stomach acid.
- Tobacco smoking. Smoking is a risk factor in that it decreases the body's response to therapy and increases changes of dying from ulcer complications, and to some extent it is a risk factor for developing an ulcer (Longe 2006). For example, smoking leads to atherosclerosis and vascular spasms, causing vascular insufficiency and promoting the development of ulcers through ischemia.
- Blood type and spices. blood group and spices, which were suspected to cause ulcers until late in the twentieth century, are actually of relatively minor importance in the development of peptic ulcers.
- Other factors. Overuse of laxatives is considered a possible cause of peptic acids. Glucocorticoids lead to atrophy of all epithelial tissues, but their role in developing ulcers is considered to be relatively small.
Symptoms and signs
Symptoms of a peptic ulcer can be:
- Abdominal pain, classically epigastric with severity relating to mealtimes, after around three hours of taking a meal (duodenal ulcers are classically relieved by food, while gastric ulcers are exacerbated by it);
- Heartburn
- Bloating and abdominal fullness
- Waterbrash (rush of saliva after an episode of regurgitation to dilute the acid in esophagus)
- Nausea, and lots of vomiting
- Loss of appetite and weight loss (gastric ulcers);
- Weight gain and pain relieved by eating (duodenal ulcers)
- Hematemesis (vomiting of blood);
- Melena (tarry, foul-smelling feces due to oxidized iron from hemoglobin passing through the rectum)
- Rarely, an ulcer can lead to a gastric or duodenal perforation. This is extremely painful and requires immediate surgery.
A history of heartburn, gastroesophageal reflux disease (GERD) and use of certain forms of medication can raise the suspicion for peptic ulcer, such as NSAIDs and glucocorticoids (e.g., dexamethasone and prednisolone).
Many individuals afflicted with stomach pain are awakened during the night. In cases of gastric ulcers, many individuals have periods of chronic pain followed by symptom-free periods that can last for several weeks or months (Longe 2006). Gastric ulcers are sometimes associated with weight loss and duodenal ulcers with weight gain (Longe 2006).
In patients over 45 with more than two weeks of the above symptoms, the odds for peptic ulceration are high enough to warrant rapid investigation by EGD (esophagogastroduodenoscopy).
Complications
About 10 to 20 percent of individuals with peptic ulcers develop complications during the illness, which can be serious (Longe 2006). Complications include:
- Perforated ulcer. Perforations are holes that develop in the duodenal or gastric wall, through which the stomach contents can lead out into the abdominal cavity (Longe 2006). May include sudden onset of the severe pain and fever, and a chemical peritonitis followed by bacterial peritonitis.
- Penetration. Penetration occurs when the ulcer erodes through the intestinal wall without digestive fluid passing into the abdomen but rather penetrating into an adjoining organ, such as the liver or pancreas (Longe 2006). Pain may be severe and radiate to the back, but be unrelated to meals.
- Hemorrhage. This is bleeding, which is the most common complication of ulcers. Mortality rate is 6 to 10 percent from hemorrhages, which can result in anemia, vomiting blood, or passage of bright red blood through the rectum (melana) (Longe 2006).
- Gastric Outlet Obstruction (Goo). This is obstruction of the digestive tract, which happens usually because of edema or scarring. It most often occurs in the outlet of the stomach in the setting of duodenal or pyloric channel ulcers. Patient may feel full after only eating a little or may have recurrent vomiting of party digested food (Longe 2006).
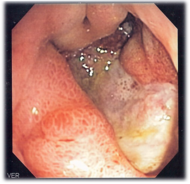
Diagnosis
An esophagogastroduodenoscopy (EGD), a form of endoscopy, also known as a gastroscopy, is carried out on patients in whom a peptic ulcer is suspected. By direct visual identification, the location and severity of an ulcer can be described. Moreover, if no ulcer is present, EGD can often provide an alternative diagnosis. If the ulcer is in the stomach, the doctor may take a tissue sample for analysis, because 3-5 percent of gastric ulcers are malignant; duodenal ulcers are rarely malignant (Longe 2006).
The diagnosis of Helicobacter pylori can be by:
- Breath testing (does not require EGD);
- Direct culture from an EGD biopsy specimen;
- Direct detection of urease activity in a biopsy specimen;
- Measurement of antibody levels in blood (does not require EGD). It is still somewhat controversial whether a positive antibody without EGD is enough to warrant eradication therapy.
The possibility of other causes of ulcers, notably malignancy (gastric cancer) needs to be kept in mind. This is especially true in ulcers of the greater (large) curvature of the stomach; most are also a consequence of chronic H. pylori infection.
Blood tests usual appear normal for ulcer patients without complications, but can be useful in evaluating anemia from an ulcer that is bleeding or show a high white blood cell count in the case of perforation or penetration (Longe 2006).
If a peptic ulcer perforates, air will leak from the inside of the gastrointestinal tract (which always contains some air) to the peritoneal cavity (which normally never contains air). This leads to "free gas" within the peritoneal cavity. If the patient stands erect, as when having a chest X-ray, the gas will float to a position underneath the diaphragm. Therefore, gas in the peritoneal cavity, shown on an erect chest X-ray or supine lateral abdominal X-ray, is an omen of perforated peptic ulcer disease.
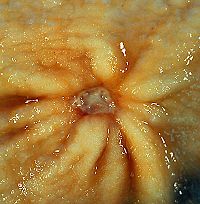
Macroscopical appearance
Gastric ulcer is most often localized on the lesser curvature of the stomach. It is a round to oval parietal defect ("hole"), 2 to 4 cm diameter, with a smooth base and perpendicular borders. These borders are not elevated or irregular as in gastric cancer - ulcerative form. Surrounding mucosa may present radial folds, as a consequence of the parietal scarring.
Microscopical appearance
Gastric peptic ulcer is a mucosal defect which penetrates the muscularis mucosae and muscularis propria, produced by acid-pepsin aggression. Ulcer margins are perpendicular and present chronic gastritis. During the active phase, the base of the ulcer shows four zones: inflammatory exudate, fibrinoid necrosis, granulation tissue and fibrous tissue. The fibrous base of the ulcer may contain vessels with thickened wall or with thrombosis (Danciu 2005).
Treatment
Medications using drugs that lower the rate of stomach acid secretions are one form of treatment, as well as drugs to protect the stomach tissues. Younger patients with ulcer-like symptoms are often treated with antacids or H2 antagonists before EGD is undertaken. Sucralfate (Carafate) helps to prevent further damage from stomach acids, as well as bismuth preparations. Bismuth compounds may actually reduce or even clear organisms.
Patients who are taking nonsteroidal anti-inflammatories (NSAIDs) may also be prescribed a prostaglandin analogue (Misoprostol) in order to help prevent peptic ulcers, which may be a side-effect of the NSAIDs.
When H. pylori infection is present, the most effective treatments are combinations of 2 antibiotics (e.g., Erythromycin, Ampicillin, Amoxicillin, Tetracycline, Metronidazole) and 1 proton pump inhibitor (PPI). An effective combination would be Amoxicillin + Metronidazole + Pantoprazole (a PPI). In the absence of H. pylori, long-term higher dose PPIs are often used.
Treatment of H. pylori usually leads to clearing of infection, relief of symptoms and eventual healing of ulcers. Recurrence of infection can occur and retreatment may be required, if necessary with other antibiotics. Since the widespread use of PPI's in the 1990s, surgical procedures (like "highly selective vagotomy," removal of part of the vagus nerve) for uncomplicated peptic ulcers became obsolete.
Perforated peptic ulcer is a surgical emergency and requires surgical repair of the perforation. Most bleeding ulcers require endoscopy urgently to stop bleeding with cautery or injection.
History
In 1997, the Centers for Disease Control and Prevention, with other U.S. government agencies, academic institutions, and industry, launched a national education campaign to inform health care providers and consumers about the link between H. pylori and ulcers. This campaign reinforced the news that ulcers are a curable infection, and the fact that health can be greatly improved and money saved by disseminating information about H. pylori (CDC 2006).
Helicobacter pylori was rediscovered in 1982 by two Australian scientists Robin Warren and Barry Marshall (Marshall 1983). Warren and Marshall (1984) contended that most stomach ulcers and gastritis were caused by colonization with this bacterium, not by stress or spicy food as had been assumed before.
The H. pylori hypothesis was poorly received, so in an act of self-experimentation Marshall drank a petri-dish containing a culture of organisms extracted from a patient and soon developed gastritis. His symptoms disappeared after two weeks, but he took antibiotics to kill the remaining bacteria at the urging of his wife, since halitosis is one of the symptoms of infection (Van der Weyden et al. 2005). In seeing what others had seen but thinking what nobody else had thought, Marshall attributes his relative inexperience in helping to think in an original way: "“If the dogma is incorrect, it’s better to know nothing about it” (Van der Weyden et al. 2005).
In 2005, the Karolinska Institute in Stockholm awarded the Nobel Prize in Physiology or Medicine to Dr. Marshall and his long-time collaborator Dr. Warren "for their discovery of the bacterium Helicobacter pylori and its role in gastritis and peptic ulcer disease."
John Lykoudis was a general practitioner in Greece who treated patients suffering from peptic ulcer disease with antibiotics long before it was commonly recognized that bacteria were a dominant cause for the disease (Rigas and Papavasassiliou 1958).
ReferencesISBN links support NWE through referral fees
- Blakemore, C., and S. Jennett. 2001. The Oxford Companion to the Body. New York: Oxford University Press. ISBN 019852403X.
- Centers for Disease Control and Prevention (CDC). 2006. Helicobacter pylori and peptic ulcer disease. Centers for Disease Control and Prevention. Retrieved July 5, 2007.
- Danciu, M. 2005. Gastric peptic ulcer. Atlas of Pathology. Retrieved July 5, 2007.
- Halpern, G. M. 2004. Ulcer Free!: Nature's Safe & Effective Remedy for Ulcers. Garden City Park, NY: Square One Publishers. ISBN 0757002536.
- Longe, J. L. 2006. The Gale Encyclopedia of Medicine. Detroit: Thomson Gale. ISBN 1414403682.
- Marshall, B. J. 1983. Unidentified curved bacillus on gastric epithelium in active chronic gastritis. Lancet 1(8336): 1273–1275. PMID 6134060.
- Marshall, B. J., and J. R. Warren. 1984. Unidentified curved bacilli in the stomach patients with gastritis and peptic ulceration. Lancet 1(8390): 1311–1315. PMID 6145023.
- Rigas, B., and E. D. Papavasassiliou. 2002. John Lykoudis. The general parctitioner in Greece who in 1958 discovered the etiology of, and a treatment for, peptic ulcer disease. In B. Marshall, ed., Helicobacter Pioneers. Firsthand accounts from the scientists who discovered helicobacters, 1892-1982. Malden, MA: Blackwell. ISBN 0867930357.
- Senior World Online (SWO). 1998. Peptic ulcers: stress does matter, after all. Senior World Online. Retrieved July 4, 2007.
- Van der Weyden, R. M. Armstrong, and A. T. Gregory. 2005. The 2005 Nobel Prize in Physiology or Medicine. Medical Journal of Australia 183(11/12): 612-614.
- Wachirawat, W., S. Hanucharurnkul, P. Suriyawongpaisal, S. Boonyapisit, S. Levenstein, J. Jearanaisilavong, K. Atisook, T. Boontong, and C. Theerabutr. 2003. Stress, but not Helicobacter pylori, is associated with peptic ulcer disease in a Thai population. J Med Assoc Thai. 86(7): 672-85.
Credits
New World Encyclopedia writers and editors rewrote and completed the Wikipedia article in accordance with New World Encyclopedia standards. This article abides by terms of the Creative Commons CC-by-sa 3.0 License (CC-by-sa), which may be used and disseminated with proper attribution. Credit is due under the terms of this license that can reference both the New World Encyclopedia contributors and the selfless volunteer contributors of the Wikimedia Foundation. To cite this article click here for a list of acceptable citing formats.The history of earlier contributions by wikipedians is accessible to researchers here:
The history of this article since it was imported to New World Encyclopedia:
Note: Some restrictions may apply to use of individual images which are separately licensed.