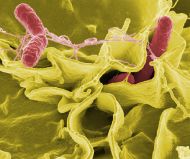
Salmonellosis
Color-enhanced scanning electron micrograph showing Salmonella typhimurium (red) invading cultured human cells | |
|---|---|
| ICD-10 | |
| ICD-O: | A02.0 |
| ICD-9 | 003.0 |
| OMIM | {{{OMIM}}} |
| MedlinePlus | 000294 |
| eMedicine | {{{eMedicineSubj}}}/{{{eMedicineTopic}}} |
| DiseasesDB | 11765 |
Salmonellosis is the name of a group of infectious diseases caused by bacteria of the genus Salmonella, including typhoid fever, paratyphoid fever, and food poisoning.
Personal and social responsibility is key in reducing the incidents of infections with salmonella. In the case of typhoid fever, transmission is tied to poor hygiene and poor public sanitation. Washing one's hands after visiting a lavatory or handling food are simple but important individual measures to reduce transmission. In the case of food poisoning, which can be contracted from improper handling and preparation of food, key steps include pasteurization of milk, treatment of public water supplies, and improvements in farm animal hygiene and vegetable and fruit harvesting and packing operations (CDC, 2006). Wider use of pasteurized eggs, education of food industry workers, improvement of restaurant inspection procedures, and even halting sale of small turtles (a common source of salmonellosis) are other valuable elements of social responsibility (CDC, 2006).
Salmonella
Salmonella are rod-shaped, gram-negative bacteria, whose main habitat is the intestinal tract of animals. As of December 7, 2005, there are two species within the genus Salmonella: Salmonella bongori (previously subspecies V) and Salmonella enterica (formerly called Salmonella choleraesuis), which is divided into six subspecies, such as Salmonella enterica subspecies enterica.
While only two species are recognized, there are numerous serotypes (or serovars). A serovar or serotype is a grouping of microorganisms (or viruses) based on their cell surface antigens, allowing differentiation below the level of species. Serovars may be established based on virulence factors, lipopolysaccharides in gram-negative bacteria, presence of an exotoxin, plasmids, or other characteristics that differentiate members of the same species (Barron, 1996). Various accounts place the number of known serotypes as "over 2,200" (Breslow, 2002) and around 4,400 (Ryan and Ray, 2004).
However, only a few of these serotypes cause infections in humans, with the majority of cases traced to only five to ten common forms (Breslow, 2002). The vast majority of human isolates (greater than 99.5 percent) are subspecies S. enterica. For the sake of simplicity, the Center for Disease Control and Prevention (CDC) recommends that Salmonella species be referred to only by their genus and serovar, for instance, Salmonella typhi, instead of the more technically correct designation, Salmonella enterica subspecies enterica serovar Typhi.
Overview of Salmonellosis
The type of salmonella usually associated with infections in humans is called Non-Typhoidal Salmonella. Food poisoning is the most common type of salmonella. It is caused by S. typhimurium or other serotypes. It is usually contracted by ingesting raw or undercooked eggs, or from improper handling of meat products. Common sources are:
- Poultry and cattle, if the meat is prepared incorrectly or becomes infected with the bacteria somehow.
- Infected eggs and milk, as well as egg products, when not prepared, handled, or refrigerated correctly.
- Reptiles such as turtles, lizards, and snakes, as they can carry the bacteria on their skin.
Non-typhoidal bacteremia (bacteræmia in British English, also known as blood poisoning or toxemia) is caused by S. enterica, S. typhimurium, or S. heidelberg in the blood.
A second, rarer general category of salmonella is called Typhoidal Salmonella. It is only carried by humans and is usually contracted through contact with the fecal matter of an infected person. It therefore mainly occurs in countries that do not have proper systems for handling human waste. This kind of salmonella infection can lead to typhoid fever.
Typhoid fever (or enteric fever) is an illness caused by the bacterium Salmonella typhi (Salmonella enterica Serovar Typhi). Common worldwide, typhoid fever is transmitted by the feco-oral route, which incorporates ingestion of food or water contaminated with feces from an infected person. Transmission involving infected urine is possible, but much less common (Giannella, 1996). According to the CDC, typhoid fever is common in most areas of the world except in industrialized regions such as the western Europe, United States, Canada, Japan, and Australia.
Paratyphoid fever is caused by infection of Salmonella paratyphi, and is also spread via the feco-oral route.
Etymology
Both Salmonellosis and the Salmonella type of microorganisms derive their names from a modern Latin coining after Daniel E. Salmon (1850–1914), an American Veterinary surgeon. He had help from Theobald Smith, and they found the bacterium in pigs in 1885.
Symptoms
In food poisoning, the bacterium induces responses in the animal that it is infecting and this is probably what causes the symptoms rather than any direct toxin. Most persons infected with Salmonella develop diarrhea, fever, vomiting, and abdominal cramps six to 72 hours after infection. Headache, fatigue, and rose spots are also possible. In most cases, the illness usually lasts three to seven days.
Most affected persons recover without treatment. However, in some persons the diarrhea may be so severe that the patient becomes dangerously dehydrated and must be taken to a hospital. At the hospital, the patients will receive intravenous fluids to treat their dehydration and medications may be given to provide symptomatic relief, like fever reduction. In severe cases, the Salmonella infection may spread from the intestines to the blood stream, and then to other body sites and can cause death unless the person is treated promptly with antibiotics. Infants, the elderly, and those with impaired immune systems are more likely to have a severe illness.
Some people afflicted with salmonellosis later experience reactive arthritis (Reiters Syndrome), which can have long-lasting, disabling effects (Dworkin et al., 2001). In sickle-cell anemia, osteomyelitis due to Salmonella infection is much more common than in the general population.
See typhoid fever for a detailed discussion of the symptoms and treatment of that disease.
Incidents of Salmonellosis
The CDC (2006) notes that about forty thousand cases of food poisoning are reported every year in the United States alone, but that mild cases are not usually reported or diagnosed and that actually cases of salmonellosis may be 30 times that number or more. Breslow (2002) notes that only an estimated one percent of cases in the United States are even reported.
One of the largest outbreaks of food poisoning occurred in the United States in 1985, when an estimated 185,000 people were infected from drinking improperly pasteurized milk (Breslow, 2002). In 1998, there were over eight hundred cases of S. enteritidis in Canada traced to a pre-packed lunch product (Breslow, 2002).
In June 2006 the British Broadcasting Company (BBC) reported that the Cadbury chocolate manufacturer withdrew a number of products because of possible contamination with salmonella (BBC, 2006). The problem had been traced to a leaking pipe at a Cadbury plant in Herefordshire in January 2006, though the announcement was not made until June.
In March 2006 the New York Times reported that the U.S. government said that 16.3 percent of all chickens were contaminated with salmonella. In the mid- to late twentieth century Salmonella enterica serovar Enteritidis was a common contaminant of eggs. This is much less common now with the advent of hygiene measures in egg production and the vaccination of laying hens to prevent salmonella colonization. Many different salmonella serovars also cause severe diseases in animals other than human beings.
Breslow (2002) reports that current concern regarding salmonellosis is centered on the emergence of multiple antibiotic resistant salmonella, which will make serious illness difficult to treat.
ReferencesISBN links support NWE through referral fees
- Baron, E.J. “Classification.” Baron's Medical Microbiology. 4th edition. University of Texas Medical Branch. 1996. ISBN 0963117211
- Breslow, L. Encyclopedia of Public Health. New York: Macmillan Reference USA/Gale Group Thomson Learning. 2002. ISBN 0028658884
- British Broadcasting Company (BBC). Cadbury recall after health fears. Retrieved November 12, 2007.
- Centers for Disease Control and Prevention. Outbreak of multidrug-resistant Salmonella Typhimurium associated with rodents purchased at retail pet stores: United States, December 2003-October 2004. Retrieved November 12, 2007.
- Centers for Disease Control and Prevention. Salmonellosis. Retrieved November 12, 2007.
- Dworkin, M.S., Shoemaker, P.C., Goldoft, M .J., and Kobayashi, J.M. “Reactive arthritis and Reiter's syndrome following an outbreak of gastroenteritis caused by Salmonella enteritidis.” Clin Infect Dis 33(7): 1010-14. 2001.
- Giannella, R.A. “Salmonella.” Baron's Medical Microbiology. 4th edition. University of Texas Medical Branch. 1996. ISBN 0963117211
- Ryan, K.J., and Ray, C.G. (ed). Sherris Medical Microbiology. 4th ed. McGraw Hill. 2004. ISBN 0838585299
Credits
New World Encyclopedia writers and editors rewrote and completed the Wikipedia article in accordance with New World Encyclopedia standards. This article abides by terms of the Creative Commons CC-by-sa 3.0 License (CC-by-sa), which may be used and disseminated with proper attribution. Credit is due under the terms of this license that can reference both the New World Encyclopedia contributors and the selfless volunteer contributors of the Wikimedia Foundation. To cite this article click here for a list of acceptable citing formats.The history of earlier contributions by wikipedians is accessible to researchers here:
The history of this article since it was imported to New World Encyclopedia:
Note: Some restrictions may apply to use of individual images which are separately licensed.