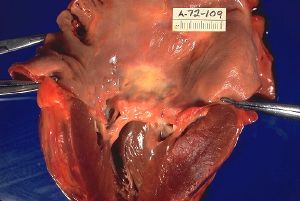
Rheumatic fever
| Rheumatic fever Classification and external resources | |
| ICD-10 | I00-I02 |
|---|---|
| ICD-9 | 390–392 |
| DiseasesDB | 11487 |
| MedlinePlus | 003940 |
| eMedicine | med/3435 med/2922 emerg/509 ped/2006 |
Rheumatic fever is an inflammatory disease that may develop after a Group A streptococcal infection (such as strep throat or scarlet fever) and can involve the heart, joints, skin, and brain. It typically arises in children as a complication of strep throat that has been untreated or inadequately treated (Longe 2006). Rheumatic fever is often characterized by arthritis (inflammation of the joints) and/or carditis (inflammation of the heart), although other symptoms may be present.
One of the most obvious preventive actions is addressing the original Group A streptococcal infection. While treatment of this infection will usually prevent progression to rheumatic fever, it is important that the full course of prescribed antibiotics be taken. One of the causal factors in progression to rheumatic fever is the premature discontinuation of the antibiotic treatment for strep throat.
Treatments of rheumatic fever include anti-inflammatory medications and antibiotics. Once one has had rheumatic fever, a course of several years of antibiotics may be needed to prevent recurrence.
General information
The Group A streptococcus bacterium (Streptococcus pyogenes, or GAS) is a form of Streptococcus bacteria responsible for most cases of streptococcal illness. Infections are largely categorized by the location of infection, including strep throat (pharynx), scarlet fever (upper body), impetigo (skin and underlying tissues). Some other diseases that can be caused by Group A streptococcus bacterium or other causal agents include pneumonia (pulmonary alveolus) and tonsillitis (tonsils).
Rheumatic fever is particularly tied to incidents of strep throat. Since children ages 5 to 15 are particularly vulnerable to strep throat, then most are susceptible to rheumatic fever (Longe 2006). Strep throat is easily treated by a ten-day course of antibiotics. However, when infection occurs without symptoms or when the medication is not taken for the full ten days, the individual has a 3 percent chance of developing rheumatic fever (Longe 2006). Rheumatic fever occurs approximately 20 days after strep throat or scarlet fever. In up to a third of cases, the underlying strep infection may not have caused any symptoms.
Rheumatic fever is common worldwide and is responsible for many cases of damaged heart valves. In the Western countries, it became fairly rare since the 1950s, probably due to widespread use of antibiotics to treat streptococcus infections. While it is far less common in the United States since the beginning of the twentieth century, there have been a few outbreaks since the 1980s. Although the disease seldom occurs, it is serious and has a mortality of 2–5 percent. Heart complications may be long-term and severe, particularly if the heart valves are involved.
In addition, persons who have suffered a case of rheumatic fever have a tendency to develop flare-ups with repeated strep infections. The recurrence of rheumatic fever is relatively common in the absence of maintenance of low dose antibiotics, especially during the first three to five years after the first episode of rheumatic fever.
Diagnosis
A list of diagnostic criteria have been developed, which were first published in 1944 by T. Duckett Jones, a medical doctor. These criteria have been periodically revised by the American Heart Association in collaboration with other groups.
These modified "Jones Criteria" are categorized into two groups: Major criteria and minor criteria. For a diagnosis of rheumatic fever, two major criteria or one major and two minor criteria have to be exhibited, and there also has to be evidence of a previous infection with with streptococcus (Longe 2006; Parrillo and Parillo 2007).
Major criteria
There are five major criteria. These are:
- Carditis. Carditis is an inflammation of the heart muscle. It can manifest as congestive heart failure with shortness of breath, pericarditis, or a new heart murmur.
- Arthritis. Arthritis, specifically migratory polyarthritis, can appear. Migratory polyarthritis is a temporary migrating inflammation of the large joints, usually starting in the legs and migrating upwards. Arthritis occurs in about 75 percent of all cases (Longe 2005).
- Cholea. Sydenham's chorea (St. Vitus' dance) is a characteristic change in coordination, such as an involuntary series of rapid movements of the face and arms without purpose. This may first be noticed as a change in handwriting, and the individual may also develop a low threshold for anger and sadness (Longe 2006). Sydenham's chorea may occur very late in the disease. It occurs in about 10 pecent of all patients (Longe 2006).
- Erythema marginatum. Erythema marginatum is a long lasting rash that begins on the trunk or arms as macules and spreads outward to form a snakelike ring, while clearing in the middle. This rash never starts on the face and is made worse with heat. *Subcutaneous nodules. Sucutaneous nodules (a form of Aschoff bodies) is a painless, firm collections of collagen fibers on the back of the wrist, the outside elbow, and the front of the knees. These now occur infrequently.
Minor criteria
There are six minor criteria that may be recognized. These are:
- Fever. Fever (temperature elevation) may occur.
- Arthralgia. Arthralgia is joint pain without swelling.
- Laboratory evidence. Such abnormalities may occur as increased erythrocyte sedimentation rate, increased C reactive protein, or leukocytosis.
- Electrical changes in the heart. Electrical changes in the heart may be observed by use of an electrocardiogram (EKG) that can measure the electrical characteristics of the heart's functioning.
- Evidence of Group A strep infection. Group A strep infection may be observed through a positive culture for Group A Strep, or elevated or rising Antistreptolysin O titre.
Other signs and symptoms include abdominal pain and nosebleeds.
Causes
Rheumatic fever is a systemic disease affecting the peri-arteriolar connective tissue, which occurs after an untreated Group A streptococcal pharyngeal infection. There are two basic theories for how the bacterial infection can lead to rheumatic fever (Longe 2006). One theory, less well supported by research, is that the bacteria produce a toxin (poisonous chemical) that circulates through the body in the bloodstream (Longe 2005). The more supported theory is that the causes is related to a problem within the body's immune system, whereby antibodies, designed to destroy invading agents, mistakenly attack the body itself, being unable to distinguish the Group A streptococcus bacteria's antigens from antigens present in the body's own cells (Longe 2006).
Specifically, it is believed that rheumatic fever is caused by antibody cross-reactivity. This cross-reactivity is a Type II hypersensitivity reaction and is termed "molecular mimicry." Usually self reactive B cells become anergic in the periphery because they fail to receive T cell co-stimulation. In the case of a strep infection, activated antigen, presenting cells against the bacterial antigen, activate helper T cells, thereby breaking the T cell anergy and subsequently B cell anergy. The B cells are now free to produce antibodies that react against the bacterial cell wall, and in addition, the mycardium and joints (Abbas and Lichtman 2004).
Group A streptococcus pyogenes has a cell wall that is composed of branched polymers, which sometimes contain "M proteins" that are highly antigenic. The antibodies the immune system generates against the "M proteins" may cross react with cardiac myofiber sarcolemma and smooth muscle cells of arteries, inducing cytokine release and tissue destruction. This inflammation occurs through direct attachment of complement and Fc receptor-mediated recruitment of neutrophils and macrophages. Characteristic Aschoff bodies, composed of swollen eosinophilic collagen surrounded by lymphocytes and macrophages can be seen on light microscopy. The larger macrophages may become Aschoff giant cells. Acute rheumatic valvular lesions may also involve a delayed hypersensitivity reaction as these lesions predominantly contain T-helper cells and macrophages (Kumar et al. 2005).
In acute rheumatic fever, these lesions can be found in any layer of the heart and is hence called pancarditis. The inflammation may cause a serofibrinous pericardial exudates described as “bread-and-butter” pericarditits, which generally resolves without sequalea. Involvement of the endocardium typically results in fibrinoid necrosis and verrucae formation along the lines of closure of the left-sided heart valves. Warty projections arise from the deposition, while subendothelial lesions may induce irregular thickenings called MacCallum plaques.
Chronic rheumatic heart disease is characterized by repeated inflammation with fibrinous resolution. The cardinal anatomic changes of the valve include leaflet thickening, commissural fusion and shortening and thickening of the tendinous cords. RHD cause 99 percent of mitral stenosis often resulting in a “fish mouth” appearance (Kumar 2005).
Treatment
The management of acute rheumatic fever is geared toward the reduction of inflammation with anti-inflammatory medications, such as aspirin or corticosteroids. Individuals with positive cultures for strep throat should also be treated with antibiotics. Another important cornerstone in treating rheumatic fever includes the continuous use of low dose antibiotics (such as penicillin, sulfadiazine, or erythromycin) to prevent recurrence.
Patients with positive cultures for streptococcus pyogenes should be treated with penicillin as long as allergy is not present. This treatment will not alter the course of the acute disease.
Patients with significant symptoms may require corticosteroids. Salicylates are useful for pain.
Some patients develop significant carditis, which manifests as congestive heart failure. This requires the usual treatment for heart failure: Diuretics, digoxin,and so forth. Unlike normal heart failure, rheumatic heart failure responds well to corticosteroids.
There are no proven effective alternative remedies for rheumatic fever, but there are some methods that may help with pain relief, cardiac function, and other symptoms (Longe 2005). Among these are massage; aramatherapy (oils of rosemary, benzoin, German chamomile, camphor, juniper, or lavender to relieve pain and oils of cypress, fennel, lemon, and wintergreen to reduce inflammation); acupuncture; and osteopathy (Longe 2005).
Prevention
The most important preventative action is addressing the original Group A streptococcal infection. Treatment of this infection with antibiotics will usually prevent progression to rheumatic fever. If an individual has a sore throat that persists longer than 24 hours, it is recommended that the person see a physician. It is important that the full course of antibiotics be taken. One of the causal factors in progression to rheumatic fever is discontinuing the antibiotics prematurely.
Prevention of recurrence is achieved by eradicating the acute infection and prophylaxis with antibiotics. A regime of antibiotics for five years or until the patient reaches 18 years of age, whichever comes first, is recommended by some practitioners (Longe 2006). The American Heart Association recommends prophylaxis continue at least 10 years.
Nurses also have a role in prevention, primarily in screening school-aged children for sore throats that may be caused by group A streptococci.
ReferencesISBN links support NWE through referral fees
- Abbas, A. K., and A. H. Lichtman. 2004. Basic Immunology: Functions and Disorders of the Immune System. Philadelphia: Saunders. ISBN 072160241X
- Ferrieri, P. 2002. Proceedings of the Jones criteria workshop. Circulation 106 : 2521–2523. Retrieved May 19, 2007.
- Jones, T. D. 1944. The diagnosis of rheumatic fever. Journal of the American Medical Association. 126: 481–484.
- Kumar, V., A. K. Abbas, N. Fausto, S. L. Robbins, and R. S. Cotran. 2005. Robbins and Cotran Pathologic Basis of Disease. Philadelphia: Elsevier Saunders. ISBN 0721601871
- Longe, J. L. 2006. The Gale Encyclopedia of Medicine. Detroit: Thomson Gale. ISBN 1414403682
- Longe, J. L. (Ed.) 2005. The Gale Encyclopedia of Alternative Medicine. Detroit: Thomson/Gale. ISBN 0787693960
- Meador, R. J., and I. J. Russell. 2005. Acute rheumatic fever. Emedicine. Retrieved May 18, 2007.
- Parrillo, S. J., and C. V. Parrillo. 2007. Rheumatic fever. Emedicine. Retrieved May 19, 2007.
External links
All links retrieved December 8, 2022.
Credits
New World Encyclopedia writers and editors rewrote and completed the Wikipedia article in accordance with New World Encyclopedia standards. This article abides by terms of the Creative Commons CC-by-sa 3.0 License (CC-by-sa), which may be used and disseminated with proper attribution. Credit is due under the terms of this license that can reference both the New World Encyclopedia contributors and the selfless volunteer contributors of the Wikimedia Foundation. To cite this article click here for a list of acceptable citing formats.The history of earlier contributions by wikipedians is accessible to researchers here:
The history of this article since it was imported to New World Encyclopedia:
Note: Some restrictions may apply to use of individual images which are separately licensed.