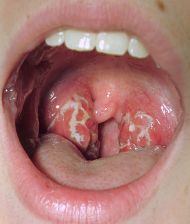
Strep throat
Strep throat | |
|---|---|
| ICD-10 | J02.0 |
| ICD-O: | {{{ICDO}}} |
| ICD-9 | 034.0 |
| OMIM | {{{OMIM}}} |
| MedlinePlus | {{{MedlinePlus}}} |
| eMedicine | {{{eMedicineSubj}}}/{{{eMedicineTopic}}} |
| DiseasesDB | {{{DiseasesDB}}} |
Strep throat, also known as Streptococcal pharyngitis or Streptococcal sore throat, is a contagious infection of the mucous membranes of the pharynx caused by group A Streptococcus bacteria. It primarily affects children and those with weakened immune systems and is responsible for about ten percent of all sore throats.
Conventional treatment of strep throat utilizing antibiotics like penicillin and erythromycin are very effective. There are also alternative treatments using goldenseal (Hydrastic canadensis), echinacea (Echinacea spp.), and garlic (Allium sativum). These, like penicillin and erythromycin, come from organisms, reflecting the rich diversity of cures available in the natural world for treating human ailments.
If strep throat is not treated, it can develop into rheumatic fever or other serious conditions. For such reasons, it is important that the full course of prescribed antibiotics be taken. One of the causal factors in progression to rheumatic fever is the premature discontinuation of the antibiotic treatment for strep throat.
Overview
Streptococcus pyogenes is a form of Streptococcus bacteria that is the primary causative agent in Group A streptococcal infections (GAS), including strep throat, acute rheumatic fever, scarlet fever, acute glomerulonephritis and necrotizing fasciitis. Infections are largely categorized by the location of infection, such as the pharynx in the case of strep throat, the upper body in the case of scarlet fever, and the skin and underlying tissues in the case of impetigo. Some other diseases that can be caused by Group A Streptococcus bacterium or other causal agents include pneumonia (pulmonary alveolus) and tonsillitis (tonsils).
Streptococcus pyogenes is a Gram-positive coccus that grows in long chains depending on the culture method (Ryan and Ray 2004). Other Streptococcus species may also possess the Group A antigen, but human infections by non-S. pyogenes GAS strains (some S. dysgalactiae subsp. equisimilis and S. anginosus Group strains) appear to be uncommon.
Strep throat is variously reported as responsible for five to ten percent of all sore throats (Longe 2006) or ten to fifteen percent of all sore throats (Longe 2005). Most sore throats are associated with viral infections such as influenza or the common cold (Longe 2006).
Strep throat primarily affects children, particularly those between the ages of 5 and 15 (Longe 2005). Others who are particular susceptible include those whose immune systems are weakened by stress or other infections, as well as smokers or those who live in damp, crowded conditions (Longe 2005; Longe 2006).
Strep throat is a contagious disease, spreading from person to person via by direct, close contact with an infected person via respiratory droplets (cough or sneezing). Rarely, food by coughing or sneezing, especially milk and milk products, can result in outbreaks.
Untreated patients are most infectious for two to three weeks after onset of infection. The incubation period, the period after exposure and before symptoms show up, is difficult to establish as some people do not become symptomatic. However, it is thought to be between two and five days.
Rheumatic fever is particularly tied to incidents of strep throat. Rheumatic fever is an inflammatory disease that may develop after a Group A streptococcal infection (such as strep throat or scarlet fever) and can involve the heart, joints, skin, and brain. It typically arises in children as a complication of strep throat that has been untreated or inadequately treated (Longe 2006). Rheumatic fever is often characterized by arthritis (inflammation of the joints) and/or carditis (inflammation of the heart), although other symptoms may be present.
Since children are particularly vulnerable to strep throat, then most are susceptible to rheumatic fever (Longe 2006). Strep throat is easily treated by a ten-day course of antibiotics. However, when infection occurs without symptoms or when the medication is not taken for the full ten days, the individual has a three percent chance of developing rheumatic fever (Longe 2006). Rheumatic fever occurs approximately 20 days after strep throat or scarlet fever. In up to a third of cases, the underlying strep infection may not have caused any symptoms.
Symptoms
The classic symptoms of strep throat are a sore throat and fever (Longe 2005). However, it is possible to have strep throat and be devoid of any of the characteristic symptoms (listed below), including not having the sore throat. Some children may complain only of a headache or stomachache (Longe 2006).
Symptoms of strep throat include:
A person with strep throat usually develops a painful sore throat and feels tired and has a fever, sometimes along with chills, headache, nausea, swollen lymph glands, and tonsils that look swollen or bright red with white or yellow patches of pus on them (Longe 2006). Often a person has bad breath. Strep throat usually does not produce the cough or runny nose characteristic of a cold or flu.
Diagnosis and tests
Initial diagnosis begins with a physical examination of the throat and chest (Longe 2006).
Two types of tests are commonly performed to see whether the patient has strep throat. The first is a rapid strep test to determine whether there is presence of Streptococcal bacteria. This test is for the presence of antibodies against the bacteria. However, this test, although fast (about ten to 20 minutes), and able to be done in the doctor's office, does not confirm whether the condition is caused by another bacteria (Longe 2006). Streptococcal bacteria may live in a person in good health, without symptoms. The rapid test has a false negative rate of about 20 percent; in other words, patients with strep throat may still yield a negative test in about 20 percent of the cases.
A second, more precise procedure is the throat culture. If the rapid test is negative, a follow-up throat culture (which takes 24 to 48 hours) may be performed. This test is very accurate and also will reveal the presence of other bacteria besides Streptococci (Longe 2006). A negative culture suggests a viral infection, in which case antibiotic treatment should be withheld or discontinued.
Predictors
A study of 729 patients with pharyngitis in which 17 percent had a positive throat culture for group A Streptococcus, identified the following four best predictors of Streptococcus (Centor et al. 1986):
1. Lack of cough
- sensitivity = 56 percent
- specificity = 74 percent
2. Swollen tender anterior cervical nodes
- sensitivity = 80 percent
- specificity = 55 percent
3. (Marked) tonsillar exudates. Although the original study did not specify the degree of exudate, "marked exudate" may be more accurate. A subsequent study of 693 patients with 9.7 percent having positive cultures found that "marked exudates" had a sensitivity and specificity of 21 percent and 70 percent while 'pinpoint exudates' were nonspecific with sensitivity and specificity of 22 percent and 45 percent (Komaroff et al. 1986).
- sensitivity = 65 percent
- specificity = 69 percent
4. History of fever
- sensitivity = 78 percent
- specificity = 45 percent
When these findings are counted in a patient, the probabilities of positive cultures in the original study (prevalence=17 percent) are (Centor et al. 1986):
- 4 findings -> 55.7 percent
- 3 findings -> 30.1 – 34.1 percent
- 2 findings -> 14.1 – 16.6 percent
- 1 findings -> 6.0 - 6.9 percent
- 0 findings -> 2.5 percent
The probabilities can also be computed with the following equation: X = −2.69 + 1.04 (exudtons) + 1 (swolacn) - 0.95 (cough) + 0.89 (fevhist)
Treatment
Antibiotic treatment will reduce symptoms slightly, minimize transmission, and reduce the likelihood of complications. Treatment consists preferably of penicillin (orally for ten days; or a single intramuscular injection of penicillin G). Erythromycin is recommended for penicillin-allergic patients. Second-line antibiotics include amoxicillin, clindamycin, and oral cephalosporins. Although symptoms subside within four days even without treatment, it is very important to start treatment within ten days of onset of symptoms, and to complete the full course of antibiotics to prevent rheumatic fever, a rare but serious complication. Other complications that can occur include an ear infection, sinus infection, acute glomerulonephritis, or an abscess on the tonsils (peritonsillar abscess).
Penicillin should be avoided for treatment of a sore throat if bacterial (swab) confirmation has not been obtained since it causes a distinctive rash if the true illness proves to be viral. This rash is harmless but alarming. The most common virus responsible for strep-like symptoms is glandular fever, also known as mononucleosis. Typically, antibiotics such as clindamycin or clarithromycin will be prescribed if there is any doubt as to whether the infection is bacterial as it does not cause a rash in the presence of a virus.
In addition to taking antibiotics, other ways to relieve strep symptoms include taking nonprescription medications (such as ibuprofen and acetaminophen/paracetamol) for throat pain and fever reduction, and getting plenty of rest. Also, gargling with warm saltwater (one-fourth teaspoon of table salt in eight oz. warm water) can help relieve throat pain as well as warm, plain tea. Avoid orange juice or other citrus drinks. The acids in them may irritate the throat.
Alternative treatments
While conventional medicine is effective in treating strep throat, several alternative therapies exist for relieving the symptoms or treating the disease (Longe 2005). Goldenseal (Hydrastic canadensis) has an alkaloid chemical, berberine, that is believed to have antibiotic effects against streptococci bacteria, and may also help to prevent S. pyogenes from attaching to the throat lining (Longe 2006). Echinacea (Echinacea spp.) is a popular herb for fighting bacterial (and viral) infections by strengthening the immune system, and may interfere with the production of an enzyme (hyaluronidase) that helps the bacterium to grow and spread (Longe 2005). Garlic (Allium sativum) is believed to have antibiotic effects. Zinc and ginger (Zingibar officinale) are used to treat symptoms of sore throat, with zinc also strengthening the immune system and reducing throat inflammation and ginger having analgesic properties.
Lack of treatment
The symptoms of strep throat usually improve even without treatment in five days, but the patient is contagious for several weeks. Lack of treatment or incomplete treatment of strep throat can lead to various complications. Some of them may pose serious health risks.
Infectious complications
- The active infection may occur in the throat, skin, and in blood.
- Skin and soft tissues may become infected, resulting in redness, pain, and swelling. Skin and deep tissues may also become necrotic (rare).
- Scarlet fever is caused by toxins released by the bacteria.
- Rarely, some strains may cause a severe illness in which blood pressure is reduced and lung injury and kidney failure may occur (toxic shock syndrome).
Noninfective complications
- During the infection, antibodies (disease–fighting chemicals) are produced.
- Rare complication can result after the organism is cleared, when these antibodies cause disease in body organs.
- Rheumatic fever is a heart disease in which the inflammation of heart muscle and scarring of heart valves can occur.
- Glomerulonephritis is a kidney disease in which the injury may lead to kidney failure.
ReferencesISBN links support NWE through referral fees
- Centor, R. M., H. P. Dalton, M. S. Campbell, M. R. Lynch, A. T. Watlington, and B. K. Garner. 1986. Rapid diagnosis of streptococcal pharyngitis in adult emergency room patients. J Gen Intern Med. 1(4): 248-251. PMID 3534175.
- Komaroff, A. L., T. M. Pass, M. D. Aronson, C. T. Ervin, S. Cretin, R. N. Winickoff, and W. T. Branch. 1986. The prediction of streptococcal pharyngitis in adults. J Gen Intern Med. 1(1): 1-7. PMID 3534166.
- Longe, J. L. 2005. The Gale Encyclopedia of Alternative Medicine. Farmington Hills, Mich: Thomson/Gale.
- Longe, J. L. 2006. The Gale Encyclopedia of Medicine. Detroit: Thomson Gale. ISBN 1414403682.
- Ryan, K. J., and C. G. Ray., eds. 2004. Sherris Medical Microbiology, 4th ed. McGraw Hill. ISBN 0838585299.
| Pathology of respiratory system (J, 460-519) | |
|---|---|
| Acute upper respiratory infections | Upper respiratory tract infection · Common cold · Rhinitis · Sinusitis · Pharyngitis (Strep throat) · Tonsillitis · Laryngitis · Tracheitis · Croup · Epiglottitis |
| Influenza and Pneumonia | Influenza · Pneumonia (Viral, Bacterial, Bronchopneumonia) |
| Other acute lower respiratory infections | Bronchitis · Bronchiolitis |
| Other diseases of upper respiratory tract | Vasomotor rhinitis · Hay fever · Atrophic rhinitis · Nasal polyp · Adenoid hypertrophy · Peritonsillar abscess · Vocal fold nodule · Laryngospasm |
| Chronic lower respiratory diseases | Emphysema · COPD · Asthma · Status asthmaticus · Bronchiectasis |
| Lung diseases due to external agents | Pneumoconiosis (Coalworker's pneumoconiosis, Asbestosis, Silicosis, Bauxite fibrosis, Berylliosis, Siderosis) · Byssinosis · Hypersensitivity pneumonitis (Farmer's lung, Bird fancier's lung) |
| Other, principally affecting the interstitium | Acute respiratory distress syndrome · Pulmonary edema · Hamman-Rich syndrome · Interstitial lung disease |
| Suppurative and necrotic conditions of lower respiratory tract | Lung abscess · Pleural effusion · Empyema |
| Other | Pneumothorax · Hemothorax · Hemopneumothorax · Mendelson's syndrome · Respiratory failure · Atelectasis · Mediastinitis |
Credits
New World Encyclopedia writers and editors rewrote and completed the Wikipedia article in accordance with New World Encyclopedia standards. This article abides by terms of the Creative Commons CC-by-sa 3.0 License (CC-by-sa), which may be used and disseminated with proper attribution. Credit is due under the terms of this license that can reference both the New World Encyclopedia contributors and the selfless volunteer contributors of the Wikimedia Foundation. To cite this article click here for a list of acceptable citing formats.The history of earlier contributions by wikipedians is accessible to researchers here:
The history of this article since it was imported to New World Encyclopedia:
Note: Some restrictions may apply to use of individual images which are separately licensed.