Hyperglycemia
Hyperglycemia, or high blood sugar, is a condition of abnormally high levels of glucose in the blood. Such excessive concentrations of blood sugar circulating in blood plasma most commonly results from type 1 or type 2 diabetes mellitus, but also can occur from other circumstances, such as illness or infection. Generally, hyperglycemia (or hyperglycaemia) is more specifically defined as any blood glucose level consistently exceeding 126 mg/dL (or 7 mmol/L). Hyperglycemia is contrasted with hypoglycemia in which blood glucose in circulating blood is consistently below 70 mg/dL (or 4 mmol/L).
Hyperglycemia represents a breakdown in the normal system that maintains glucose levels within an acceptable range. It is a treatable condition, but if not addressed it can develop into one of two life-threatening complications: diabetic ketoacidosis (DKA) or hyperglycemic hyperosmolar nonketotic syndrome (HHNS).
Overview
Blood glucose levels need to be maintained within a narrow range, despite the impact of consuming substantial carbohydrates or considerable intervals between meals. Normally, these blood glucose levels are maintained by two complementary groups of metabolic hormones. Insulin, an anabolic polypeptide hormone synthesized in the pancreas, regulates carbohydrate metabolism such as to decrease blood glucose. The catabolic hormones (such as glucagon, growth hormone, and catecholamines) increase blood glucose.
Various conditions can affect the level of blood glucose levels above or below the normal range. One of the most well-known of these is diabetes mellitus, a condition where there is abnormally high blood glucose levels. The two most common forms of diabetes are due to either a diminished production of insulin (in type 1), or diminished response by the body to insulin (in type 2 and gestational). Both lead to hyperglycemia, which largely causes the acute signs of diabetes: excessive urine production, resulting compensatory thirst and increased fluid intake, blurred vision, unexplained weight loss, lethargy, and changes in energy metabolism. Patients with type 1 diabetes mellitus depend on external insulin for their survival because of an absolute deficiency of the hormone. Patients with type 2 diabetes mellitus have insulin resistance or relatively low insulin production, or both; some type 2 diabetics eventually require insulin when other medications become insufficient in controlling blood glucose levels.
Hyperglycemia results when there is an abundance of glucose in the bloodstream, such as when the glucose in the blood cannot enter cells. The hyperosmolar, glucose-rich blood draws fluid from the intracellular and interstitial spaces and causes thirst and dehydration (Fain 2001). Chronic hyperglycemia can result when diabetes is untreated or poorly controlled, while acute hyperglycemia can result when there is an underlying condition that interferes with glucose control, such as an illness or infection, as well as those with type 2 diabetes that are under extreme stress (Fain 2001).
The term hyperglycemia comes from the Greek hyper, meaning "excessive," -glyc-, meaning "sweet," and -emia, meaning "of the blood."
Measurement and definition
Glucose levels are measured in either:
- Milligrams per deciliter (mg/dL), in the United States and other countries (e.g., Japan, France, Egypt, Colombia); or
- Millimoles per liter (mmol/L), which can be acquired by dividing (mg/dL) by factor of 18.
Scientific journals are moving towards using mmol/L; some journals now use mmol/L as the primary unit but quote mg/dL in parentheses.
Comparatively:
|
|
|
Glucose levels vary before and after meals, and at various times of day; the definition of "normal" varies among medical professionals. In general, the normal range for most people (fasting adults) is about 80 to 120 mg/dL or 4 to 7 mmol/L. A subject with a consistent range above 126 mg/dL or 7 mmol/L is generally held to have hyperglycemia, whereas a consistent range below 70 mg/dL or 4 mmol/L is considered hypoglycemic. In fasting adults, blood plasma glucose should not exceed 126 mg/dL or 7 mmol/L. Sustained higher levels of blood sugar cause damage to the blood vessels and to the organs they supply, leading to the complications of diabetes.
Chronic hyperglycemia can be measured via the HbA1c test. The definition of acute hyperglycemia varies by study, with mmol/L levels from 8 to 15 (Giugliano et al. 1997;
Causes
Diabetes mellitus
Chronic hyperglycemia that persists even in fasting states is most commonly caused by diabetes mellitus, and in fact chronic hyperglycemia is the defining characteristic of the disease. Acute episodes of hyperglycemia without an obvious cause may indicate developing diabetes or a predisposition to the disorder. This form of hyperglycemia is caused by low insulin levels. These low insulin levels inhibit the transport of glucose across cell membranes therefore causing high blood glucose levels.
Eating disorders and medications
Certain eating disorders can produce acute non-diabetic hyperglycemia, as in the binge phase of bulimia nervosa, when the subject consumes a large amount of calories at once, frequently from foods that are high in simple and complex carbohydrates. Certain medications also increase the risk of hyperglycemia, including beta blockers, thiazide diuretics, corticosteroids, niacin, pentamidine, protease inhibitors, L-asparaginase (Detin et al. 1994), and some antipsychotic agents (Luna and Feinglos 2001).
Times of physiologic stress
A high proportion of patients suffering an acute stress such as stroke or myocardial infarction may develop hyperglycemia, even in the absence of a diagnosis of diabetes. Human and animal studies suggest that this is not benign, and that stress-induced hyperglycemia is associated with a high risk of mortality after both stroke and myocardial infarction (Capes et al. 2001).
Hyperglycemia occurs naturally during times of infection and inflammation. When the body is stressed, endogenous catecholamines are released that, among other things, serve to raise the blood glucose levels. The amount of increase varies from person to person and from inflammatory response to response. As such, no patient with first-time hyperglycemia should be diagnosed immediately with diabetes if that patient is concomitantly sick. Further testing, such as a fasting plasma glucose, random plasma glucose, or two-hour postprandial plasma glucose level, must be performed.
A transient hyperglycemic episode also can be triggered by a stress that overtaxes a person’s mental resources (Culvert 2005).
Symptoms
The following symptoms may be associated with acute or chronic hyperglycemia, with the first three comprising the classic hyperglycaemic triad:
- Polyphagia - frequent hunger, especially pronounced hunger
- Polydipsia - frequent thirst, especially excessive thirst
- Polyuria - frequent urination, especially excessive urination
- Blurred vision
- Fatigue
- Weight loss
- Poor wound healing (cuts, scrapes, etc.)
- Dry mouth
- Dry or itchy skin
- Impotence (male)
- Recurrent infections such as vaginal yeast infections, groin rash, or external ear infections (swimmer's ear)
- Kussmaul hyperventilation: deep, rapid breathing
- Cardiac arrhythmia
- Stupor
- Coma
Frequent hunger without other symptoms can also indicate that blood sugar levels are too low. This may occur when people who have diabetes take too much oral hypoglycemic medication or insulin for the amount of food they eat. The resulting drop in blood sugar level to below the normal range prompts a hunger response. This hunger is not usually as pronounced as in Type I diabetes, especially the juvenile onset form, but it makes the prescription of oral hypoglycemic medication difficult to manage.
Polydipsia and polyuria occur when blood glucose levels rise high enough to result in excretion of excess glucose via the kidneys (glycosuria), producing osmotic diuresis.
Symptoms of acute hyperglycemia may include:
- Ketoacidosis
- A decreased level of consciousness or confusion
- Dehydration due to glycosuria and osmotic diuresis
- Acute hunger and/or thirst
- Impairment of cognitive function, along with increased sadness and anxiety (Pais et al. 2007; Sommerfield et al. 2004)
Treatment and prognosis
Treatment of hyperglycemia requires elimination of the underlying cause, such as treatment of diabetes when diabetes is the cause or removal of stressors. Acute and severe hyperglycemia can be treated by direct administration of insulin in most cases, under medical supervision. Treatment of hyperglycemia should be done with close monitoring and delivered carefully in order to avoid the risk of hypokalemia (higher than normal blood serum levels of potassium) and subsequent edema (Culvert 2005).
The prognosis for individuals with mild to moderate hyperglycemia is good, based on treatment. Severe hyperglycemia, with glucose levels in the blood serum in the range of 800 mg/dL, can lead to cerebral edema, coma, and death if not treated promptly (Culvert 2005).
ReferencesISBN links support NWE through referral fees
- Capes, S. E., D. Hunt, K. Malmberg, P. Pathak, and H. C. Gerstein. 2001. Stress hyperglycemia and prognosis of stroke in nondiabetic and diabetic patients: A systematic overview Stroke 32(10): 2426–32. PMID 11588337. Retrieved September 21, 2008.
- Cetin, M., S. Yetgin, A. Kara, et al. 1994. Hyperglycemia, ketoacidosis and other complications of L-asparaginase in children with acute lymphoblastic leukemia. J Med 25(3-4): 219–29. PMID 7996065. Retrieved September 21, 2008.
- Culvert, L. L. 2005. Hyperglycemia. In K. M. Krapp, and J. Wilson, The Gale Encyclopedia of Children's Health: Infancy Through Adolescence. Detroit: Thomson Gale. ISBN 0787692417.
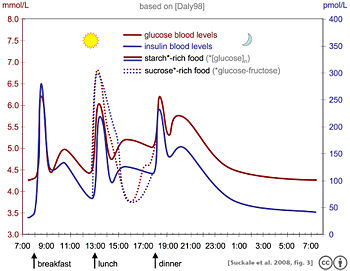
- Daly, M. E., C. Vale, M. Walker, A. Littlefield, K. G. Alberti, and J. C. Mathers. 1998. Acute effects on insulin sensitivity and diurnal metabolic profiles of a high-sucrose compared with a high-starch diet Am J Clin Nutr. 67(6): 1186-96. Retrieved September 21, 2008.
- Fain, J. A. 2001. Lowering the boom on hypoglycemia Springhouse Corporation. Retrieved September 21, 2008.
- Giugliano, D., R. Marfella, L. Coppola, et al. 1997. Vascular effects of acute hyperglycemia in humans are reversed by L-arginine. Evidence for reduced availability of nitric oxide during hyperglycemia Circulation 95(7): 1783–90. PMID 9107164. Retrieved September 21, 2008.
- Luna, B., and M. N. Feinglos. 2001. Drug-induced hyperglycemia JAMA 286(16): 1945–8. PMID 11667913.
- Pais, I., M. Hallschmid, K. Jauch-Chara, et al. 2007. Mood and cognitive functions during acute euglycaemia and mild hyperglycaemia in type 2 diabetic patients Exp. Clin. Endocrinol. Diabetes 115(1): 42–6. PMID 17286234. Retrieved September 21, 2008.
- Sommerfield, A. J., I. J. Deary, and B. M. Frier. 2004. Acute hyperglycemia alters mood state and impairs cognitive performance in people with type 2 diabetes Diabetes Care 27(10): 2335–40. PMID 15451897. Retrieved September 21, 2008.
Credits
New World Encyclopedia writers and editors rewrote and completed the Wikipedia article in accordance with New World Encyclopedia standards. This article abides by terms of the Creative Commons CC-by-sa 3.0 License (CC-by-sa), which may be used and disseminated with proper attribution. Credit is due under the terms of this license that can reference both the New World Encyclopedia contributors and the selfless volunteer contributors of the Wikimedia Foundation. To cite this article click here for a list of acceptable citing formats.The history of earlier contributions by wikipedians is accessible to researchers here:
The history of this article since it was imported to New World Encyclopedia:
Note: Some restrictions may apply to use of individual images which are separately licensed.